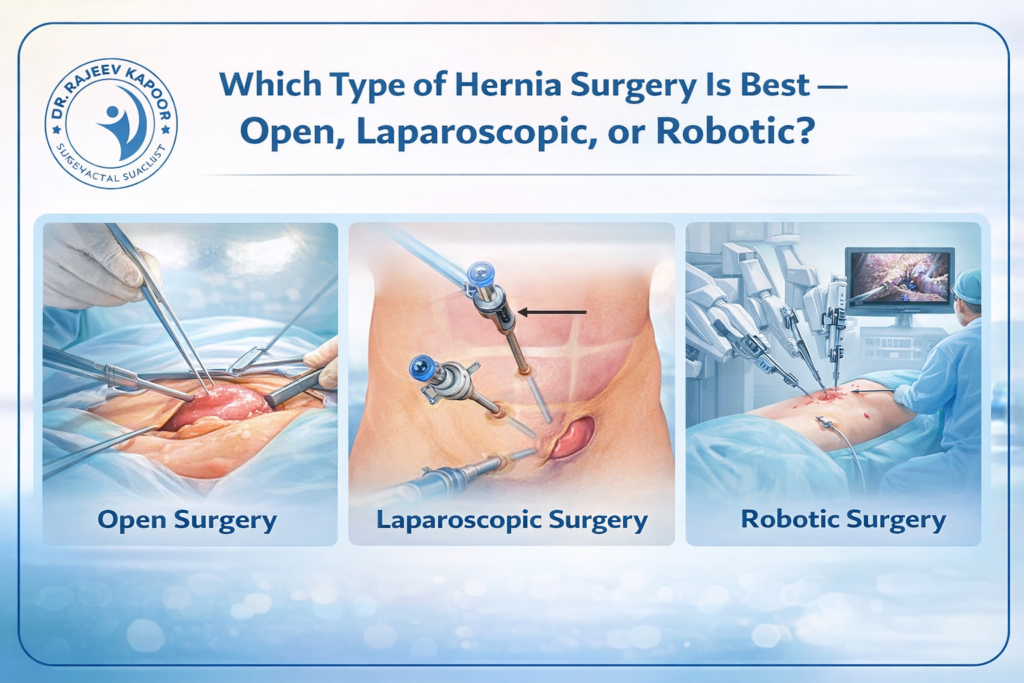
Which Type of Hernia Surgery Is Best — Open, Laparoscopic, or Robotic?
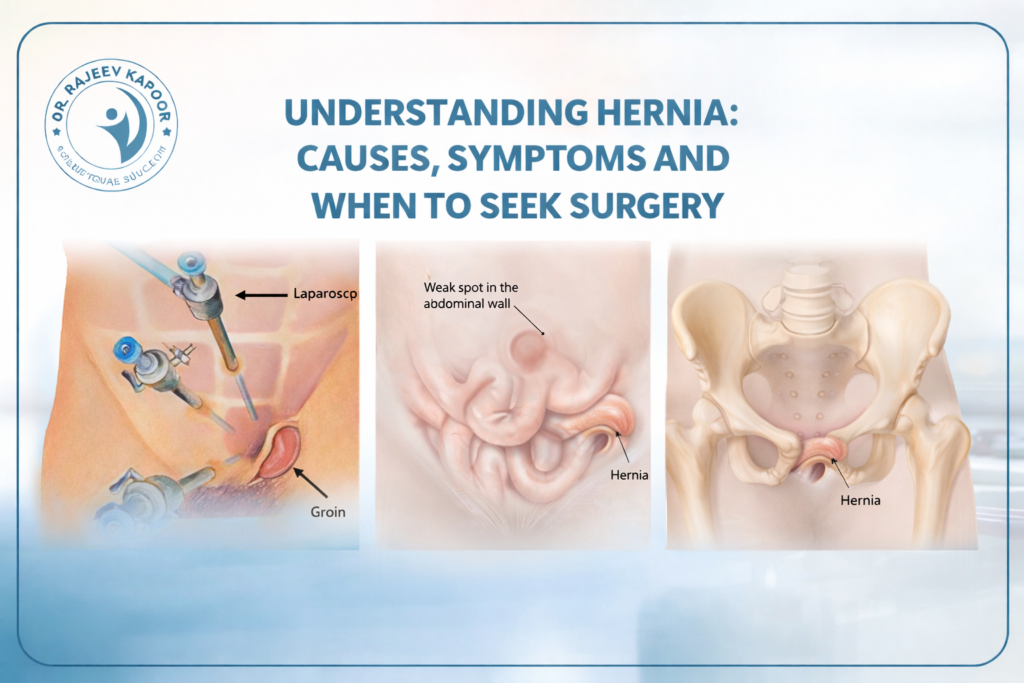
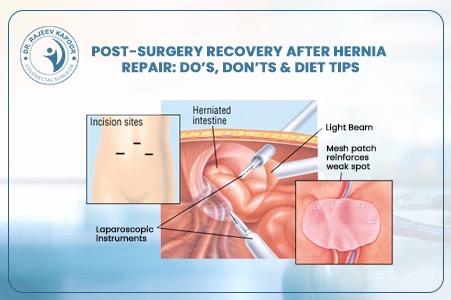
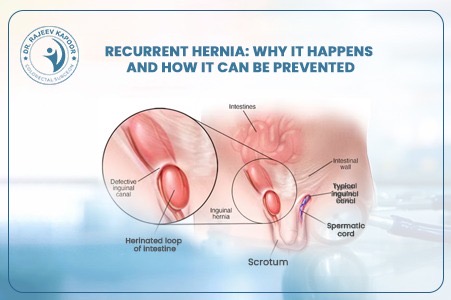
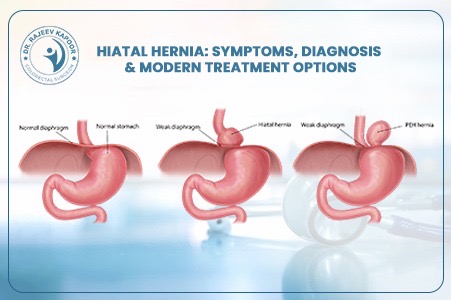
With over 30 years of surgical experience, Dr. Rajeev Kapoor has managed a wide spectrum of abdominal wall hernias using both conventional and advanced minimally invasive techniques. One of the most common concerns patients have after diagnosis is: “Which type of hernia surgery is best — open, laparoscopic, or robotic?” The answer is not universal. The ideal technique depends on the type of hernia, its size, previous surgeries, patient health status, and surgical expertise. This article explains each option clearly so you can make an informed decision. What Is a Hernia? A hernia occurs when an internal organ or tissue protrudes through a weakened area of the abdominal wall. The most common types include: 1. Inguinal Hernia Occurs in the groin region and is more common in men. 2. Umbilical Hernia Appears near the belly button. 3. Incisional Hernia Develops at the site of a previous surgical incision. 4. Ventral Hernia Occurs anywhere along the abdominal wall. Hernias do not resolve on their own. Surgery is the only definitive treatment to prevent complications such as obstruction or strangulation. Types of Hernia Surgery Explained 1️⃣ Open Hernia Surgery How It Is Performed A single incision is made directly over the hernia site. The protruding tissue is pushed back into the abdominal cavity, and a surgical mesh is placed to reinforce the weakened muscle wall. Advantages Suitable for large or complicated hernias Can be performed under spinal or local anesthesia Cost-effective Widely available Limitations Slightly larger incision Longer recovery compared to minimally invasive techniques Higher immediate post-operative discomfort When Is Open Surgery Preferred? Very large incisional hernias Patients unfit for general anesthesia Strangulated or emergency hernias Open repair remains a reliable and time-tested procedure with excellent long-term outcomes when performed properly. 2️⃣ Laparoscopic Hernia Surgery How It Is Performed Three small keyhole incisions are made. A camera (laparoscope) provides magnified internal visualization, and specialized instruments repair the defect using mesh placement from inside the abdomen. Advantages Smaller scars Reduced post-operative pain Faster recovery Early return to work Lower infection risk Ideal For Bilateral inguinal hernias Recurrent hernias after open repair Patients seeking faster recovery Recovery Most patients resume routine activities within 7–10 days. Laparoscopic surgery in Chandigarh has become increasingly preferred for suitable candidates due to quicker rehabilitation. 3️⃣ Robotic Hernia Surgery How It Is Performed This technique uses a robotic surgical platform controlled entirely by the surgeon. It provides high-definition 3D visualization and enhanced precision in suturing and mesh placement. Advantages Superior dexterity and precision Better visualization of complex defects Potentially less post-operative pain Improved outcomes in complex abdominal wall reconstruction Considerations Higher procedural cost Requires specialized infrastructure Not necessary for all simple hernias Robotic surgery is particularly beneficial in complex or recurrent hernias where fine dissection is critical. Key Factors That Determine the Best Approach Choosing the best hernia surgery involves evaluating: Type and size of hernia Primary or recurrent Previous abdominal surgeries Patient’s age and comorbidities (diabetes, obesity, cardiac issues) Risk of anesthesia Surgeon’s experience An individualized surgical plan ensures optimal results and minimizes recurrence. What About Mesh — Is It Safe? Modern hernia repairs typically involve placement of a synthetic mesh to strengthen the abdominal wall. When performed correctly: Recurrence rates are significantly reduced Long-term durability improves Complication rates remain low Concerns about mesh are usually related to improper technique or infection — not the material itself. Recovery After Hernia Surgery Recovery depends on the technique used: Surgery Type Hospital Stay Return to Work Pain Level Open 1–2 days 2–4 weeks Moderate Laparoscopic 24 hours 7–10 days Mild Robotic 24 hours 7–10 days Mild Patients are advised to avoid heavy lifting for 4–6 weeks irrespective of the approach. Which Surgery Is Best for You in Chandigarh? There is no universally “best” technique. The best option is the one that: Addresses your specific hernia type Minimizes complications Offers durable repair Matches your medical profile An experienced general surgeon evaluates these factors clinically before recommending a surgical plan. When Should You Not Delay Surgery? Seek prompt evaluation if you experience: Sudden severe pain Vomiting with abdominal swelling Redness over hernia site Inability to push the hernia back These may indicate strangulation — a surgical emergency. Conclusion Hernia surgery has evolved significantly. While open surgery remains dependable, laparoscopic and robotic techniques offer faster recovery and improved cosmetic outcomes in suitable patients. The most important factor is not the technology — it is proper surgical judgment and experience. If you are considering hernia surgery in Chandigarh, a detailed clinical evaluation will determine the safest and most effective treatment plan tailored specifically to you.