Surgical Management of Cancer
Understanding the role of surgery in cancer care — conditions treated, surgical approaches, and the multidisciplinary team that guides treatment.
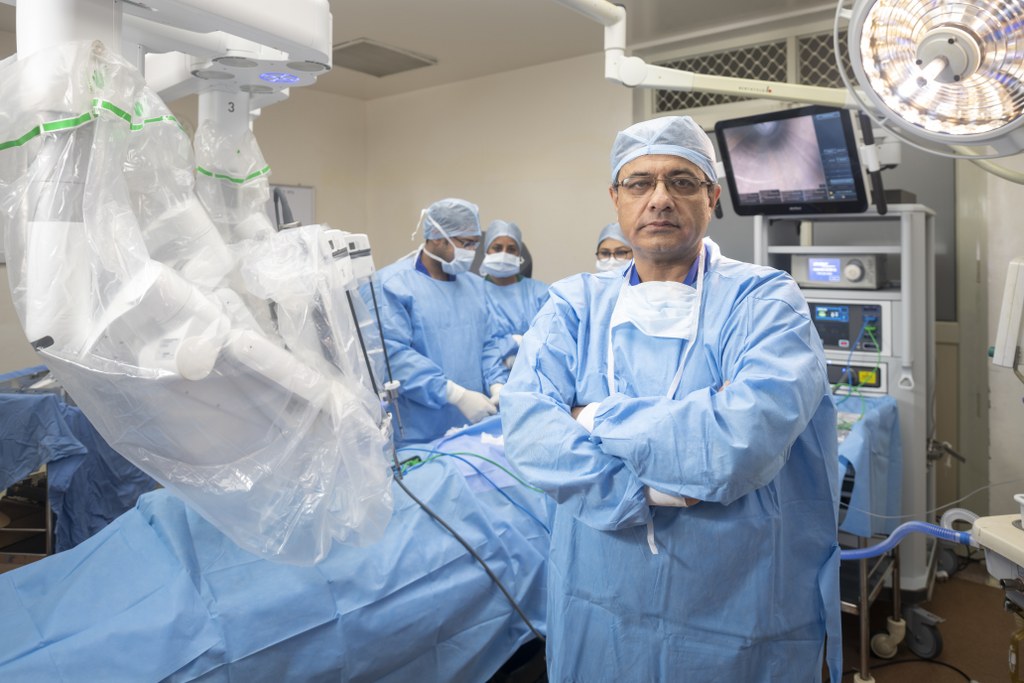
About Cancer Surgery
Surgery is the primary treatment for many cancers, particularly those involving the digestive tract and reproductive organs. This page explains which cancers may need surgery, what that surgery involves, and how treatment decisions are made — in plain language, for patients and families.
How this page helps you: Whether you have received a cancer diagnosis, are accompanying a family member, or want to understand your options — this resource explains surgical treatment in clear, accessible language. It does not replace a personal consultation with your surgeon or oncologist.
Cancer surgery at Fortis Hospital Mohali is delivered through a structured multidisciplinary team → About Dr. Kapoor — surgeons, oncologists, radiologists, and pathologists — who review every case together before a plan is finalised.

Cancers Requiring Surgical Management
The following cancers commonly require surgical assessment and treatment. For each, a brief explanation of the condition, its symptoms, and how surgery fits into the overall plan is provided.
Colon Cancer → Colorectal Cancer
Cancer of the large intestine (colon) is one of the most common cancers worldwide. It typically arises from polyps — small growths on the inner lining of the colon — that gradually become malignant over years.
- Often develops without symptoms in early stages
- Symptoms may include change in bowel habit, blood in stools, unexplained weight loss, or abdominal discomfort
- Diagnosed via colonoscopy → Colonoscopy Guide, biopsy, CT scan, and staging investigations
- Surgery is the primary treatment for resectable colon cancer
- Procedures: right hemicolectomy, left hemicolectomy, sigmoid colectomy
- Laparoscopic (keyhole) and robotic approaches are available for suitable patients
Rectal Cancer → Colorectal Cancer
Cancer arising in the rectum — the last segment of the large intestine — requires particularly careful surgical planning due to the rectum's proximity to the anal sphincter, bladder, and reproductive organs.
- Symptoms: rectal bleeding, altered bowel habit, tenesmus (feeling of incomplete emptying), pelvic pain
- Investigations: MRI of the pelvis is essential for staging and surgical planning
- Pre-operative chemotherapy and radiotherapy are often used to shrink the tumour before surgery
- Total Mesorectal Excision (TME) → Open Surgery is the surgical gold standard
- Sphincter-preserving surgery is performed wherever oncologically safe
- Robotic surgery offers precision in the confined pelvic space
Cancer of the Anal Canal
Cancer of the anal canal is less common than colon or rectal cancer. It is often treated first with chemotherapy and radiotherapy (chemoradiation), with surgery reserved for specific situations.
- Symptoms: anal bleeding, pain, change in bowel habit, a palpable mass
- Strongly associated with HPV infection in some cases
- Chemoradiation is the first-line treatment for most squamous cell carcinomas of the anal canal
- Surgery (abdominoperineal resection) may be required if chemoradiation fails or for adenocarcinoma
- Surgical management requires close coordination with the medical oncology and radiation oncology teams
Cancer of the Appendix
Appendix cancer is rare and often discovered incidentally during or after surgery for appendicitis. The most common type is a carcinoid (neuroendocrine tumour) or a mucinous tumour.
- Often asymptomatic until discovered during appendicectomy
- Mucinous tumours may cause pseudomyxoma peritonei — spread of mucous material in the abdomen
- Treatment depends on tumour size, type, and extent of spread
- Small carcinoids (<2 cm) may be adequately treated by appendicectomy alone
- Larger or more aggressive tumours require right hemicolectomy
- Advanced cases with peritoneal spread may require HIPEC → Open Surgery & HIPEC combined with cytoreductive surgery
A dedicated article on appendiceal cancer is available in the → Patient Learning Centre.
Ovarian Cancer
Ovarian cancer often presents at an advanced stage because early-stage disease may be asymptomatic. Surgery is central to both diagnosis and treatment.
- Symptoms: abdominal bloating, early satiety, pelvic discomfort, urinary changes
- Investigations: pelvic ultrasound, CA-125 blood test, CT scan
- Surgery aims to remove as much tumour as possible (cytoreductive surgery / debulking) → Open Surgery
- Standard procedure involves removal of both ovaries and fallopian tubes, uterus, omentum, and affected lymph nodes
- When the bowel is involved, colorectal surgical expertise is required for bowel resection and reconstruction
- Chemotherapy (usually platinum-based) follows surgery
Vulvar Cancer
Vulvar cancer is a relatively uncommon gynaecological malignancy but requires precise surgical planning due to the anatomy of the region and the need for functional preservation and reconstruction.
- Symptoms: persistent vulvar itching, pain, a lump, or skin changes
- Treatment for resectable tumours is surgical excision with appropriate margins
- Wide local excision or radical vulvectomy depending on extent
- Sentinel lymph node biopsy and inguinal lymphadenectomy may be required
- Reconstruction may be needed following extensive resection
Skin Cancers & Soft Tissue Tumours
Skin cancers range from the highly common and readily treatable to the more aggressive forms that require careful surgical planning. Surgical excision is the cornerstone of treatment for most skin malignancies.
- Squamous Cell Carcinoma (SCC): arises from the outer layers of skin; requires wide local excision with adequate margins; lymph node assessment if high-risk features are present
- Basal Cell Carcinoma (BCC): the most common skin cancer; rarely spreads but can be locally destructive if untreated; treated by surgical excision, often with primary reconstruction
- Melanoma: the most serious form of skin cancer; treatment involves wide excision with margins determined by tumour thickness (Breslow depth); sentinel lymph node biopsy (SLNB) → Open Surgery is performed for appropriate staging
- Merkel Cell Carcinoma: a rare but aggressive neuroendocrine skin cancer requiring wide excision, lymph node evaluation, and often adjuvant radiation
- Reconstruction following skin cancer excision — flaps, grafts, or primary closure — is planned to achieve both oncological safety and optimal functional and cosmetic outcome
Abdominal & Retroperitoneal Sarcomas
Soft tissue sarcomas arising in the abdomen and retroperitoneum are rare but can grow to considerable size before diagnosis. Complete surgical resection offers the best chance of disease control.
- May present as a palpable abdominal mass, vague discomfort, or incidentally on imaging
- CT and MRI are essential for pre-operative planning
- Goal of surgery is complete resection with clear margins (R0 resection) → Open Surgery
- Adjacent organ involvement (bowel, kidney, vessels) may require en bloc resection
- Multidisciplinary planning is essential — treatment decisions require input from oncology, radiology, and pathology
The Role of Surgery in Cancer Treatment
Surgery can play several roles in cancer treatment — depending on the cancer type, its stage, and what the overall plan requires. Understanding these roles helps patients and families prepare.
Curative Surgery
When cancer is confined to one location and has not spread to other organs or distant lymph nodes, complete surgical removal may be curative. This is the goal in most early-stage colorectal → Colorectal Cancer and gynaecological cancers. The extent of surgery depends on the location, size, and biological behaviour of the tumour.
Surgery After Neoadjuvant Therapy
For some cancers — particularly rectal cancer and locally advanced ovarian cancer — chemotherapy and/or radiotherapy is given before surgery to shrink the tumour. This neoadjuvant approach may also allow sphincter-preserving surgery → Surgical Techniques in rectal cancer cases where the tumour was initially too close to the anal sphincter.
Surgery as Part of Combined Treatment
Many cancers are treated with a combination of surgery, chemotherapy, and radiation therapy. Surgery removes the primary tumour while additional treatments address microscopic spread and reduce the risk of recurrence. Sequence and type of treatments are decided by the multidisciplinary team.
Cytoreductive Surgery
In cancers such as advanced ovarian cancer or appendiceal cancer with peritoneal spread, the goal of surgery may be debulking — removing as much tumour as possible to improve the effectiveness of subsequent chemotherapy. This is often combined with HIPEC → Open Surgery & HIPEC.
Emergency Surgery for Cancer Complications
Occasionally, a cancer may present as a surgical emergency — most commonly bowel obstruction or perforation from colorectal cancer → Colorectal Cancer. Emergency surgery addresses the immediate complication and may or may not include definitive cancer surgery depending on the patient's condition.
Important: The decision to proceed with surgery is always made following a thorough clinical assessment, appropriate investigations, and an informed discussion with the patient. No two patients are the same, and treatment recommendations are individualised accordingly.
Surgical Approaches Used in Cancer Surgery
Modern cancer surgery offers several approaches. The right choice depends on the cancer type and stage, the patient's overall fitness, and the anatomy involved. Keyhole techniques are used wherever they are safe and effective.
🤖 Robotic Surgery
Robot-assisted surgery provides three-dimensional vision and highly articulated instruments that work with precision in confined spaces such as the pelvis — particularly valuable in rectal cancer and gynaecological cancer surgery. Recovery is generally faster with fewer complications compared to open surgery → Open Surgery.
Learn more about robotic surgery🔑 Laparoscopic Surgery
Laparoscopic (keyhole) surgery uses small incisions through which a camera and instruments are passed. It is the standard of care for suitable colon cancer → Colorectal Cancer operations and offers reduced pain, shorter hospital stay, and faster return to normal activity compared to open surgery.
Learn more about laparoscopic surgery⚕️ Open Surgery
Open surgery — using a standard abdominal incision — remains the appropriate choice in certain situations: very large tumours, extensive peritoneal spread, previous major abdominal surgery, or when the anatomy requires direct access → Open Surgery in Cancer. Open surgery is not inferior to keyhole surgery when performed carefully by an experienced team.
🎯 Total Mesorectal Excision (TME)
TME is the surgical gold standard for rectal cancer → Rectal Cancer. It involves precise removal of the rectum along with its surrounding fatty tissue envelope (mesorectum) — where lymph nodes and potential cancer spread reside. TME significantly reduces local recurrence rates and is performed both laparoscopically and robotically.
💠 Sphincter-Preserving Surgery
Maintaining normal bowel continuity — and avoiding a permanent colostomy → Living with a Stoma — is a priority wherever oncologically safe. Advances in surgical technique and neoadjuvant therapy have made it possible to preserve the sphincter in many rectal cancers that previously required permanent stoma formation.
Learn more about sphincter-preserving surgery🧪 HIPEC (Hyperthermic Intraperitoneal Chemotherapy)
For selected cases of appendiceal cancer or colorectal cancer with peritoneal spread, cytoreductive surgery combined with HIPEC — delivery of heated chemotherapy directly into the abdominal cavity — may be considered. This is a major operation requiring careful patient selection → Open Surgery & HIPEC.
A detailed, plain-language explanation of all surgical techniques is available in the → Surgical Techniques Explained section of the Patient Learning Centre.
For a focused overview of colorectal conditions and surgery, see the Colorectal Surgery → Colorectal Surgery page.
Multidisciplinary Cancer Care
For most cancers, the best results come when specialists across disciplines work together on a shared plan. At Fortis Hospital Mohali, every complex cancer case is reviewed by a multidisciplinary team (MDT) before treatment begins.
Treatment plans are discussed in MDT meetings before being finalised. Patients are provided with a clear explanation of the recommended approach, the rationale for treatment decisions, and the opportunity to ask questions before giving informed consent.

What to Expect — The Care Pathway
Knowing what to expect — from diagnosis through surgery and recovery — helps reduce anxiety and lets patients and families prepare. Below is a general overview of the care pathway.
Clinical Assessment & Investigations
A thorough history and examination is performed, followed by appropriate investigations — which typically include blood tests, colonoscopy → Colonoscopy Guide or endoscopy, CT scan, MRI, and PET-CT scan depending on the cancer type and suspected stage.
MDT Discussion & Treatment Planning
Once investigations are complete, the case is discussed within the multidisciplinary team. A treatment plan is formulated — which may involve surgery alone, or surgery in combination with chemotherapy and/or radiation therapy in a defined sequence.
Informed Consent & Pre-operative Preparation
The proposed surgery is explained in full — its purpose, what it involves, possible risks and complications, expected recovery, and alternatives. Pre-operative preparation may include bowel preparation, stopping certain medications, and nutritional optimisation.
→ Before & After Surgery GuideSurgery
The operation is performed in a modern modular operating theatre under general anaesthesia. The anaesthetic team monitors the patient throughout. Duration varies significantly depending on the complexity of the procedure — from 2 hours for a straightforward laparoscopic colectomy to 8+ hours for cytoreductive surgery with HIPEC → Open Surgery.
Post-operative Care & Recovery
Recovery begins in the post-operative ward or ICU depending on the magnitude of surgery. Pain management, physiotherapy, and nutritional support are provided. Hospital stay varies from 3–10 days for most colorectal procedures. Discharge criteria include satisfactory wound healing, adequate oral intake, and return of bowel function.
→ What to expect after surgeryPathology Review & Adjuvant Treatment
The removed specimen is sent for detailed pathological analysis — which confirms the diagnosis, assesses surgical margins, and determines the final cancer stage. This information guides decisions about adjuvant (post-operative) chemotherapy or radiation.
Follow-up & Surveillance
After cancer surgery, regular follow-up is essential to monitor for recurrence, manage late effects, and support overall wellbeing. Follow-up schedules include clinical review, blood tests (tumour markers such as CEA for colorectal cancer), and periodic imaging. Colonoscopy surveillance → Colonoscopy Guide is part of standard follow-up for colorectal cancer. Family screening may also be recommended → Screening & Prevention.
Related Information
Explore further educational resources on this website:
Have Questions?
If you have received a diagnosis and would like to understand your options, or if you have been referred for a surgical opinion, details of how to reach the clinical team at Fortis Hospital Mohali are on the contact page.
Contact Information
Professional Disclosure & Disclaimer (NMC Compliant):
This page is maintained for the purpose of patient education and factual information. It does not constitute medical advice, a diagnosis, or a treatment recommendation. Surgical treatment decisions are made individually, following clinical assessment by a qualified medical team. No comparative claims are made and no specific outcomes are guaranteed. Dr. Rajeev Kapoor practises as Additional Director, Oncology & Colorectal Surgery at Fortis Hospital, Sector 62, Phase 8, Mohali — an NABH-accredited institution.
For appointments or enquiries: Contact page | drrajeevkapoor.com

