Cancer Can Be Found Before You Feel It
Most cancers cause no symptoms in the early stages — but they can still be detected. Screening saves lives. Find out which test you need, at what age, and how often.
Why Should I Get Screened?
This is the most important thing to understand: cancer in its early stages causes no symptoms. You feel completely normal. You eat normally, work normally, and have no pain. But the cancer is growing quietly.
"I have seen patients whose cancer was caught early by chance — or by screening — and they went home completely cured. I have also seen patients who came in with advanced disease because they waited for symptoms that never appeared early. Screening is the single most important step you can take."
— Dr. Rajeev Kapoor, MS, Colorectal Fellowship (Australia)
Colorectal & Cancer Surgeon
Screening means testing people who feel perfectly well, before any symptoms develop. The logic is straightforward: the earlier a cancer is found, the smaller it is, the less it has spread, and the easier it is to treat — or remove completely.
For colorectal cancer, screening does something even more powerful. The colon does not jump straight from healthy tissue to cancer. It almost always passes through a middle stage: a polyp. A polyp is a small, harmless-looking growth that can, over 5–15 years, slowly turn cancerous. A colonoscopy finds these polyps and removes them in the same procedure — before they become cancer. This is why colorectal cancer screening can actually prevent the disease, not just detect it early.
For breast and cervical cancer, the same principle applies: early detection means smaller tumours, less aggressive treatment, and far better outcomes. For cervical cancer, HPV vaccination combined with regular screening can eliminate the disease almost entirely.

Source: SEER database, IARC, Indian Cancer Registry. All figures approximate 5-year relative survival rates.
The pattern is the same for every cancer: catch it at Stage I — survival is high. Wait for symptoms to appear — survival drops sharply. Screening is the difference between the two.
⚠️ Warning Signs — When to See a Doctor
These symptoms do not always mean cancer — but they must always be checked. Do not assume rectal bleeding is "just piles." Do not ignore unexplained weight loss. A proper examination is the only way to be sure.
Blood in the Stool
Blood mixed in stool, on the toilet paper, or in the toilet bowl. Even bright red bleeding needs examination — never assume it is just haemorrhoids without a check-up.
Sudden, Unexplained Weight Loss
Losing 4–5 kg or more in a few weeks without trying — no diet change, no illness. This needs urgent investigation.
Severe or Worsening Abdominal Pain
New pain in the abdomen that keeps getting worse, or pain accompanied by vomiting and inability to pass stool. Go to hospital today.
Coughing or Vomiting Blood
Blood in vomit, or blood when you cough (especially with chest pain or breathlessness). This always needs same-day assessment.
Change in Bowel Habits > 3 Weeks
New pattern of diarrhoea, constipation, or alternating between the two that is unusual for you. A feeling that your bowel does not empty fully.
Unexplained Tiredness or Anaemia
Persistent fatigue not explained by your lifestyle, or a blood test showing low haemoglobin with no obvious cause. This can be a sign of slow internal bleeding.
Narrow or Ribbon-Like Stools
Stools that have become persistently thinner or flatter than normal. This can indicate a narrowing in the bowel caused by a growth.
Loss of Appetite or Nausea
Unexplained loss of appetite, persistent nausea, or difficulty eating — especially when combined with other bowel symptoms or weight loss.
Lump in the Abdomen or Rectum
Any new lump felt in the abdomen or around the anal area, or a feeling of pressure or a mass inside the rectum.
Persistent Cough or Hoarse Voice
A cough or hoarseness lasting more than 3 weeks, especially in smokers. Can be a sign of lung or throat cancer. Needs a check-up.
Breast Lump or Nipple Change
Any new breast lump, change in breast shape, skin dimpling, or unusual nipple discharge in women (or men). Always needs prompt assessment.
Abnormal Vaginal Bleeding
Bleeding between periods, after intercourse, or after menopause in women. Can be a sign of cervical or uterine cancer. See a gynaecologist.
Having one or more of these symptoms does not mean you have cancer. Most of the time there is a simple, benign explanation — haemorrhoids, irritable bowel, a viral infection, or stress. But the only way to be certain is a proper examination. Early assessment is always the right decision — and the reassurance it gives is itself valuable.
Each of these symptoms is usually innocent — many have common, benign explanations. But when persistent for more than 2–3 weeks, they must be investigated.
Rectal bleeding is the most dismissed symptom in bowel cancer. Most people assume haemorrhoids — and most of the time they are right. But the only way to be certain is a proper examination. If you are over 40, or have any other symptom alongside bleeding, a colonoscopy is the appropriate investigation.
Unexplained weight loss triggers systematic investigation including blood tests, imaging, and endoscopy. Do not rationalise it without checking.
Change in bowel habit sustained over 3+ weeks is a red flag, especially combined with bleeding. The combination in anyone over 40 is a strong indicator for colonoscopy.
📅 No symptoms? Build your personal screening calendar — add recurring phone reminders for every test you need.
Plan My Screening →📋 Cancer Screening Schedule — Which Test, At What Age, How Often
Use this as your personal screening checklist. The right test depends on your age, gender, and whether cancer runs in your family. If you are not sure, speak to a doctor — a simple conversation can save your life.
Your Cancer Screening Guide — At a Glance
Based on international guidelines adapted for India. Family history changes everything — if cancer runs in your family, you may need to start earlier.
| Cancer | Who Should Screen | When to Start | Test | How Often | Available In India |
|---|---|---|---|---|---|
|
🔴
Bowel (Colorectal) Cancer
Average Risk
|
Men & Women with no family history of bowel cancer |
45 yrs
Continue until age 75
|
FIT Stool Test — simple home test for hidden blood in stool OR Colonoscopy — camera check of entire bowel |
FIT test: Every year Colonoscopy: Every 10 years if result is normal |
✅ Private |
|
🔴
Bowel Cancer
Family History
|
Parent, sibling, or child had bowel cancer or large polyps |
40 yrs
Or 10 yrs before relative's diagnosis age
|
Colonoscopy — stool tests alone are not enough for high-risk patients | Every 3–5 years (not 10) | ✅ Private |
|
🧬
Bowel Cancer
Lynch / FAP
|
Known Lynch syndrome or FAP gene carrier |
20–25 yrs
As directed by specialist
|
Colonoscopy — annual or every 1–2 years | Every 1–2 years | 🏥 Specialist |
|
🎗️
Breast Cancer
Average Risk
|
All women; earlier if mother/sister had breast cancer |
40 yrs
Clinical exam from 25–30
|
Mammography — breast X-ray Clinical breast examination by doctor from age 25 |
Every 1–2 years |
✅ Free (CBE) ✅ Private (Mammo) |
|
🧬
Breast Cancer
BRCA Carrier
|
Known BRCA1 or BRCA2 gene mutation carrier |
25–30 yrs
|
Annual Mammography + Breast MRI | Every year | 🏥 Specialist |
|
💜
Cervical Cancer
All Women
|
All sexually active women; HPV vaccine recommended girls 9–14 |
25 yrs
Until age 65
|
Pap Smear (cytology) from age 25 HPV + Pap co-test from age 30 |
Pap smear: Every 3 years HPV + Pap: Every 5 years |
✅ Free (VIA) ✅ Private (Pap) |
|
🔵
Prostate Cancer
Men Only
|
Men aged 50+; age 45 if father or brother had prostate cancer |
50 yrs
45 if family history
|
PSA Blood Test — discuss results with urologist; not all raised PSA means cancer | Every 1–2 years (discuss with urologist) | ✅ Private |
|
🫁
Lung Cancer
Heavy Smokers
|
Heavy smokers or ex-smokers (20+ pack-years); age 50–80 |
50 yrs
Smokers only; discuss with doctor
|
Low-Dose CT Scan (LDCT) — not a standard chest X-ray | Every year | ✅ Private |
|
🫀
Stomach Cancer
High Risk
|
Family history of gastric cancer, H. pylori infection, chronic gastritis |
45 yrs
Or if symptoms appear
|
Upper Endoscopy (Gastroscopy) + H. pylori test | As advised by specialist | ✅ Private |
|
👄
Oral Cancer
Tobacco Users
|
Tobacco, pan, betel nut, or alcohol users; anyone with a mouth ulcer lasting >3 weeks |
30 yrs
Or earlier if tobacco use
|
Oral Visual Inspection — by a dentist or health worker | Every year |
✅ Free ✅ Private |
Important: This table is a general guide. Your personal screening plan should be decided with your doctor based on your age, gender, and family history. If cancer has occurred in more than one family member, or at a young age, please seek a specialist opinion — you may need to start screening much earlier.
For more information, contact your doctor. You can also contact Dr. Kapoor directly.
Contact Dr. Kapoor →📅 Your Personal Screening Calendar
Enter your details. I'll show which tests apply to you, when to start, and how often — and you can add a recurring reminder to your iPhone, Android, Google Calendar, or Outlook with one tap. It repeats automatically — you never need to remember again.
Note: This tool gives general guidance based on established screening guidelines and Dr. Kapoor's clinical recommendations. Your individual plan may differ based on your medical history — use this as a starting point for a discussion with your doctor.
Bowel (Colorectal) Cancer Screening
Bowel cancer is one of the most common cancers in India — and one of the most preventable. A colonoscopy can not only detect cancer early, it can remove pre-cancerous polyps before they ever turn into cancer.
Who Needs Bowel Cancer Screening?
No Family History
Men and women with no relatives who had bowel cancer.
Start at age 45
Colonoscopy every 10 years if normal; or FIT stool test yearly
Family History
A parent, sibling, or child had bowel cancer or large polyps.
Start at age 40
Or 10 years before the age your relative was diagnosed — colonoscopy every 3–5 years
Inherited Syndrome
Lynch syndrome, FAP, or long-standing IBD (Crohn's / Ulcerative Colitis) affecting the colon.
Start in teens / early 20s
Personalised plan from your specialist — every 1–2 years
What Are the Tests?
Colonoscopy
A camera is gently passed through the bowel under sedation. The doctor can both see and remove any polyps in one sitting. Most patients go home the same day.
FIT Stool Test
No preparation, no sedation. You collect a small stool sample at home and send it to a lab. If blood is detected, a colonoscopy is needed. A good first step if you are nervous about a scope.
CT Colonography
A special CT scan of the bowel — sometimes called "virtual colonoscopy". No sedation is needed. If polyps are found, a standard colonoscopy is still needed to remove them.
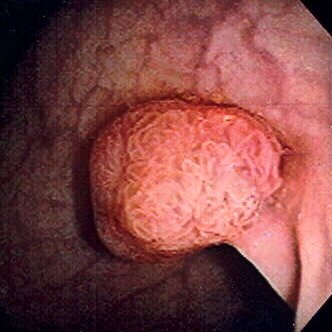
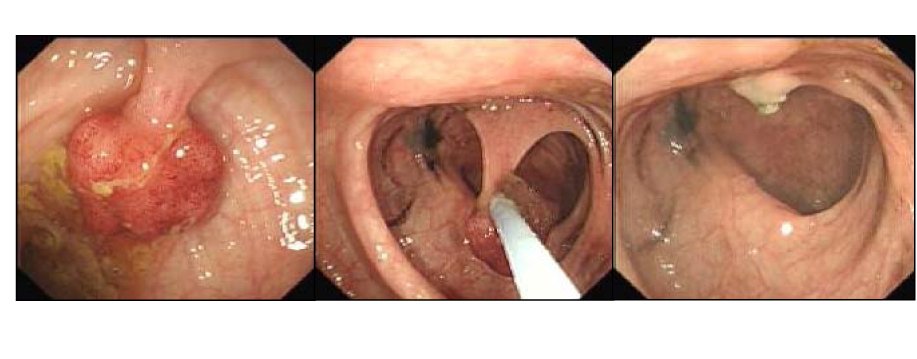
What happens during a colonoscopy?
You will be asked to clear your bowel the day before using a preparation drink. On the day, you will receive a mild sedative — you will be comfortable and relaxed, but awake. A flexible camera (colonoscope) is gently passed through your rectum and guided along the full length of the large bowel.
The whole procedure takes about 30–45 minutes. If any polyps are seen, they are removed at the same time using a small wire loop — painlessly. You are monitored for about an hour afterwards and go home the same day.
Common questions about colonoscopy
🧬 Cancer in the Family — What It Means for You
If your parent, sibling, or child has had cancer, your own risk may be significantly higher — and your screening should start earlier. In some families, cancer is caused by a gene that is passed from parent to child. This is called hereditary or familial cancer.
If two or more close relatives have had the same type of cancer, or if cancer appeared at a young age (under 50), this is a warning sign. You should discuss genetic testing and earlier screening with a specialist. Do not wait until you get symptoms.
Lynch Syndrome
Lynch syndrome is passed down in families as an autosomal dominant condition — meaning one faulty copy of the gene (from either parent) is enough to significantly raise your risk. Not everyone who carries the gene will get cancer, but the risk is high enough to warrant regular surveillance.
If Lynch syndrome is identified in your family, all first-degree relatives (parents, siblings, children) should be offered genetic testing. This is a blood test that looks for the specific gene change. Genetic counselling — a specialist consultation before and after the test — is strongly recommended.
Genetic testing for Lynch syndrome is available at major cancer centres in Chandigarh and Delhi. Speak to your colorectal surgeon or oncologist for a referral.
Familial Adenomatous Polyposis (FAP)
FAP is rarer than Lynch syndrome but carries a very high cancer risk if not managed. Because the condition is almost certain to lead to cancer if left untreated, surgery to remove the colon (colectomy) is nearly always recommended.
The type of surgery depends on the number and location of polyps and the patient's age. Options include total colectomy with ileorectal anastomosis (bowel reconnected to the rectum, which must still be monitored) or a restorative proctocolectomy with ileal pouch (J-pouch). This is a complex surgical decision that should be made with an experienced colorectal surgeon.
BRCA1 & BRCA2 Gene Mutations
BRCA mutations are not rare — approximately 1 in 400 people in the general population carries a BRCA mutation, and the frequency is even higher in certain groups. Identifying a BRCA mutation in one family member means that all first-degree relatives can be offered testing.
For men with BRCA mutations, the risk of prostate cancer is also significantly elevated. BRCA2 carriers have an approximately 20% lifetime risk of prostate cancer (vs ~10% in the general population), and PSA testing should begin earlier — from age 45.
Risk-reducing surgery (prophylactic mastectomy, prophylactic oophorectomy) is an option for women with BRCA mutations. This is a major personal decision that requires detailed discussion with an experienced multidisciplinary team including a breast surgeon, gynaecological oncologist, and genetic counsellor.
Hereditary Diffuse Gastric Cancer (HDGC)
Hereditary diffuse gastric cancer is rare but particularly difficult to manage because the cancer does not form a visible lump — it spreads through the stomach wall in what is called a "linitis plastica" pattern. Standard endoscopy often misses early disease, which is why annual gastroscopy with a very specific multi-site biopsy protocol is used for surveillance.
Because surveillance may not reliably detect early cancer, many specialists and patients opt for prophylactic gastrectomy. This means removing the stomach before cancer develops. People can live well after a total gastrectomy with dietary modifications, though it is a significant adjustment. A specialist centre experienced in managing hereditary gastric cancer should be consulted.
Should My Family Be Tested?
If you have a personal or family history of cancer — especially at a young age, or the same cancer in multiple relatives — speak to your doctor about genetic counselling and testing. A referral can be made to a clinical geneticist or a cancer genetics clinic at a major centre in Chandigarh or Delhi.
Genetic testing is a blood or saliva test. Results typically take 4–8 weeks. Before and after testing, you will meet with a genetic counsellor who can explain what the results mean for you and your family.
A positive result does not mean you will definitely get cancer — it means your risk is higher, and you need more frequent, earlier screening. In some cases, preventive surgery may be an option.
For more information, contact your doctor. You can also contact Dr. Kapoor directly.
Contact Dr. Kapoor →Screening for Other Common Cancers
While my main specialty is colorectal cancer, I regularly see patients with concerns about other cancers. Here is a plain-language guide to screening for the most common cancers in India — please consult the relevant specialist for your personal plan.
Lung Cancer Private Only
Lung cancer is the leading cause of cancer death worldwide. Most cases are found late — when symptoms like persistent cough, blood in sputum, or chest pain have already appeared. Smokers are at much higher risk.
- Annual LDCT scan recommended for heavy smokers aged 50–80 (20+ pack-years of smoking)
- Not recommended for non-smokers without symptoms or high-risk features
- Quitting smoking is the single most effective thing you can do — risk drops significantly within 5–10 years of stopping
A pack-year is calculated as: number of packs smoked per day × number of years smoked. So 1 pack per day for 20 years = 20 pack-years. This is the threshold at which annual LDCT is recommended internationally. The test is a quick, low-radiation CT scan of the chest — it is not the same as a regular chest X-ray, which is much less sensitive for early lung cancer.
Stomach (Gastric) Cancer Private Only
Stomach cancer is more common in India than in Western countries and is often diagnosed late. Warning signs include persistent indigestion, difficulty swallowing, upper abdominal pain, and feeling full very quickly.
- Upper endoscopy (gastroscopy) is the main test for upper digestive symptoms
- Testing and treating H. pylori infection significantly reduces gastric cancer risk — a simple breath test or stool antigen test can detect this common stomach bacteria
- High-risk individuals: strong family history, previous gastric polyps, chronic gastritis, long-term use of acid-suppressing medication
Helicobacter pylori (H. pylori) infection is found in approximately 40–50% of the Indian population. Not everyone who has it gets cancer, but treatment of H. pylori with a short course of antibiotics significantly reduces the risk of developing gastric cancer — this is a simple and highly effective intervention.
Breast Cancer ✅ NPCDCS Programme
Breast cancer is the most common cancer in Indian women. When found at an early, localised stage, survival rates are over 95%. Regular mammography from age 40 can catch cancer before a lump can be felt.
- Mammography (breast X-ray) from age 40–50 — every 1–2 years. Discuss timing with your gynaecologist.
- Clinical breast examination (CBE) by a doctor from age 25–30
- Women with a BRCA1/2 mutation or strong family history need annual mammography AND breast MRI from age 25–30
- Breast self-examination monthly helps you notice changes between clinical screenings
Mammography finds breast cancers when they are smaller and more treatable — often before they can be felt as a lump. For most women, annual mammography starting at 40 strikes the right balance.
High-risk women (BRCA1/2 mutation or strong family history) need annual mammography AND breast MRI from age 25–30. MRI is more sensitive for dense breast tissue and picks up what mammography can miss.
BRCA genetic testing is now available in India. If your mother, sister, or daughter had breast or ovarian cancer — especially at a young age — genetic counselling is appropriate. A positive BRCA result changes your screening schedule and may prompt preventive options.

Cervical Cancer ✅ NPCDCS Programme
Cervical cancer is the 2nd most common cancer in Indian women — and it is almost entirely preventable with HPV vaccination and regular screening. This is one cancer where screening truly eliminates the disease.
- Pap smear (cervical cytology) every 3 years from age 25 to 65
- HPV test + Pap co-testing every 5 years from age 30 is more sensitive
- HPV vaccination — girls aged 9–14 ideally (up to 26) — is highly effective at preventing infection with the viruses that cause 70%+ of cervical cancers
- Warning signs that need urgent assessment: abnormal vaginal bleeding, bleeding after sex, post-menopausal bleeding, or unusual vaginal discharge
Cervical cancer has a long pre-cancer phase — abnormal cells (called CIN) can be detected years before becoming invasive cancer. A Pap smear picks these up. Treatment of CIN is a simple outpatient procedure. This is why cervical cancer is almost entirely preventable.
HPV causes over 99% of cervical cancers. The HPV vaccine (Cervarix or Gardasil) given to girls aged 9–14 before first sexual exposure provides near-complete protection. India's national programme now provides HPV vaccination free to girls aged 9–14.
A Pap smear + HPV co-test every 5 years from age 30 is more sensitive than a Pap smear alone. Women who have had a total hysterectomy for a non-cancerous reason with no CIN history no longer need cervical screening — discuss with your gynaecologist.
Prostate Cancer Private Only
Prostate cancer is the 2nd most common cancer in men worldwide. It is often slow-growing and may cause no symptoms for years. When found early, it is highly treatable — most men are cured.
- PSA (Prostate Specific Antigen) blood test — discuss with your urologist from age 50 (age 45 if a father or brother had prostate cancer)
- A raised PSA does not automatically mean cancer — it needs specialist interpretation
- Digital rectal examination (DRE) remains an important part of the assessment
- Warning signs: difficulty starting urination, weak flow, blood in urine or semen, frequent night urination, pelvic pain
PSA (Prostate Specific Antigen) is a simple blood test measuring a protein made by the prostate. An elevated PSA can indicate cancer — but can also be raised by benign enlarged prostate (BPH), prostatitis, or even vigorous exercise. Specialist interpretation is needed.
The benefit: PSA can detect prostate cancer when still confined to the gland and most curable. When it spreads to lymph nodes or bone, treatment becomes far more complex.
The limitation: PSA can lead to finding very slow-growing cancers that may never cause harm in a man's lifetime — this is called over-diagnosis. The decision to screen should be made with your doctor, factoring in your age, overall health, and your preferences.
Men with a first-degree relative (father, brother) who had prostate cancer should consider screening from age 45. The PSA test is simple — the conversation about what to do next is the important step.
Note: For cancers other than colorectal, please consult the relevant specialist — a gynaecologist, oncologist, pulmonologist, or urologist. I am happy to assist with a referral from my clinic at Fortis Hospital Mohali.
What Increases Your Risk of Bowel Cancer?
Some risk factors you cannot change — your age, your genes, your family history. But several important risk factors can be changed, and reducing them can significantly lower your cancer risk.
⚠️ Risk Factors You Cannot Change
- Age over 45 — risk increases steadily with age, most cases occur in people over 50
- Family history — a parent, sibling, or child with bowel cancer or large polyps doubles your risk
- Inherited syndromes — Lynch syndrome, FAP, or MUTYH-associated polyposis
- Personal history of bowel cancer or advanced polyps previously
- Long-standing inflammatory bowel disease — Crohn's or Ulcerative Colitis affecting the colon for 8+ years
- Previous pelvic radiotherapy for another cancer
✅ Risk Factors You CAN Change
- Low-fibre diet — eat more vegetables, fruits, whole grains, dal, and sabzi. Reduce processed and red meat.
- Obesity — maintaining a healthy weight significantly reduces bowel cancer risk
- Physical inactivity — aim for 30 minutes of moderate exercise, 5 days a week
- Smoking — smokers have a significantly higher risk. Quitting helps at any age.
- Heavy alcohol — more than 2 standard drinks a day raises risk. Limit consumption.
- Type 2 diabetes — associated with moderately increased bowel cancer risk; managing blood sugar helps
Indian diet and bowel cancer risk
Traditional Indian diets — rich in vegetables, legumes (dal, channa, rajma), whole grains (roti, jowar, bajra), and spices — are actually highly protective against bowel cancer. The problem is urbanisation. As more Indians shift to fast food, processed meats, white rice, and low-fibre packaged foods, bowel cancer rates are rising.
Protective foods: leafy vegetables (palak, methi), legumes (dal, rajma, chole), whole grains, turmeric, garlic, and onions. Foods to limit: processed meats, red meat (limit to 2–3 times a week), refined carbohydrates, and sugary drinks.
Exercise and cancer prevention
Physical activity reduces bowel cancer risk by approximately 24% in the most active individuals compared to the least active. The mechanism includes effects on insulin levels, bile acid metabolism, bowel transit time, and inflammation.
You do not need to run marathons. 30 minutes of brisk walking, cycling, or swimming — 5 days a week — is enough to significantly reduce your risk. Even standing and moving regularly throughout the day helps.
📅 Ready to plan your screening from now through the next decade? Build your personal calendar.
Build My Calendar →For More Information, Contact Your Doctor
The recommendations on this page are based on established screening guidelines and Dr. Kapoor's clinical practice. Every person's screening needs are different — your age, family history, and risk factors all matter. For personalised advice, please speak with your doctor.
You can also contact Dr. Kapoor directly for more information.
Colorectal · Cancer · General Surgery | Chandigarh · Mohali · Panchkula
Frequently Asked Questions
Common questions I am asked about cancer screening in India — answered plainly.
At what age should I start bowel cancer screening in India?
If you have no family history of bowel cancer, start at age 45. If a parent, sibling, or child has had bowel cancer, start at age 40 — or 10 years before the age at which your relative was diagnosed. People with Lynch syndrome or FAP should start in their early 20s or even teens. If you are not sure, ask your doctor.
I feel completely fine. Do I still need screening?
Yes — this is exactly when screening works best. Bowel cancer and polyps cause no symptoms in the early stages. By the time symptoms appear, the cancer may have already progressed. Most patients found to have early bowel cancer through screening say they felt perfectly normal. Feeling well is not a reason to skip screening.
Is colonoscopy painful? I am scared of the procedure.
Colonoscopy at Fortis Hospital Mohali is done with sedation — you will be comfortable and relaxed throughout. Most patients feel very little or no pain. Some mild bloating or cramping for an hour or two afterwards is normal. The preparation (clearing the bowel the day before) is the part most patients find unpleasant, but it is manageable. The benefits far outweigh the temporary discomfort.
My mother had breast cancer. What should I do?
Start by discussing your family history with a specialist. If your mother was diagnosed before age 50, or if multiple relatives on the same side of the family have had breast cancer, you may benefit from genetic counselling and testing for BRCA mutations. Even without a gene mutation, a first-degree relative with breast cancer means you should start mammography earlier — discuss the timing with your gynaecologist or oncologist.
What is Lynch syndrome and should my family be tested?
Lynch syndrome is the most common inherited bowel cancer condition. It is caused by a change in one of four genes (MLH1, MSH2, MSH6, PMS2). People with Lynch syndrome have a 40–80% lifetime risk of bowel cancer. If bowel cancer has occurred at a young age in your family, or in multiple relatives, ask your doctor about genetic testing. If Lynch syndrome is confirmed, all first-degree relatives should be offered testing. Colonoscopy every 1–2 years from age 20–25 is the recommended surveillance.
Is cancer screening free in India?
The government's NPCDCS programme offers free screening for cervical cancer (VIA test), breast cancer (clinical breast examination), and oral cancer at government Health and Wellness Centres for adults aged 30–65. Bowel cancer screening is not included in this programme and is only available in the private sector. A FIT stool test is the lowest-cost private option.
How do I know if I have H. pylori? Does it cause cancer?
H. pylori is a bacteria found in the stomach of approximately 40–50% of Indians. Most people have no symptoms. H. pylori is a significant risk factor for stomach cancer — infection causes chronic inflammation that, over many years, can lead to cancer. A simple breath test or stool antigen test can detect H. pylori. If positive, a 2-week course of antibiotics clears the infection and significantly reduces your cancer risk. Ask your doctor for an H. pylori test if you have persistent indigestion or a family history of stomach cancer.
Did You Know? Cancer Screening in India
The honest picture — why screening in India matters more than many people realise.
India's annual colorectal cancer burden — the 4th most common cancer in the country (GLOBOCAN 2022).
93% of people who should be screened for bowel cancer in India are not. Most are diagnosed at an advanced stage.
Urban Chandigarh has nearly 2–3× the bowel cancer incidence of rural Punjab — westernised diet is a key driver.
The NPCDCS programme covers these at government Health and Wellness Centres for adults aged 30–65.
Stage I bowel cancer has a 90%+ survival rate. Found at Stage IV it drops to around 10–15%. Late diagnosis is the problem.
Find the polyp, remove it during colonoscopy, and the cancer never develops. Screening at the right time works.