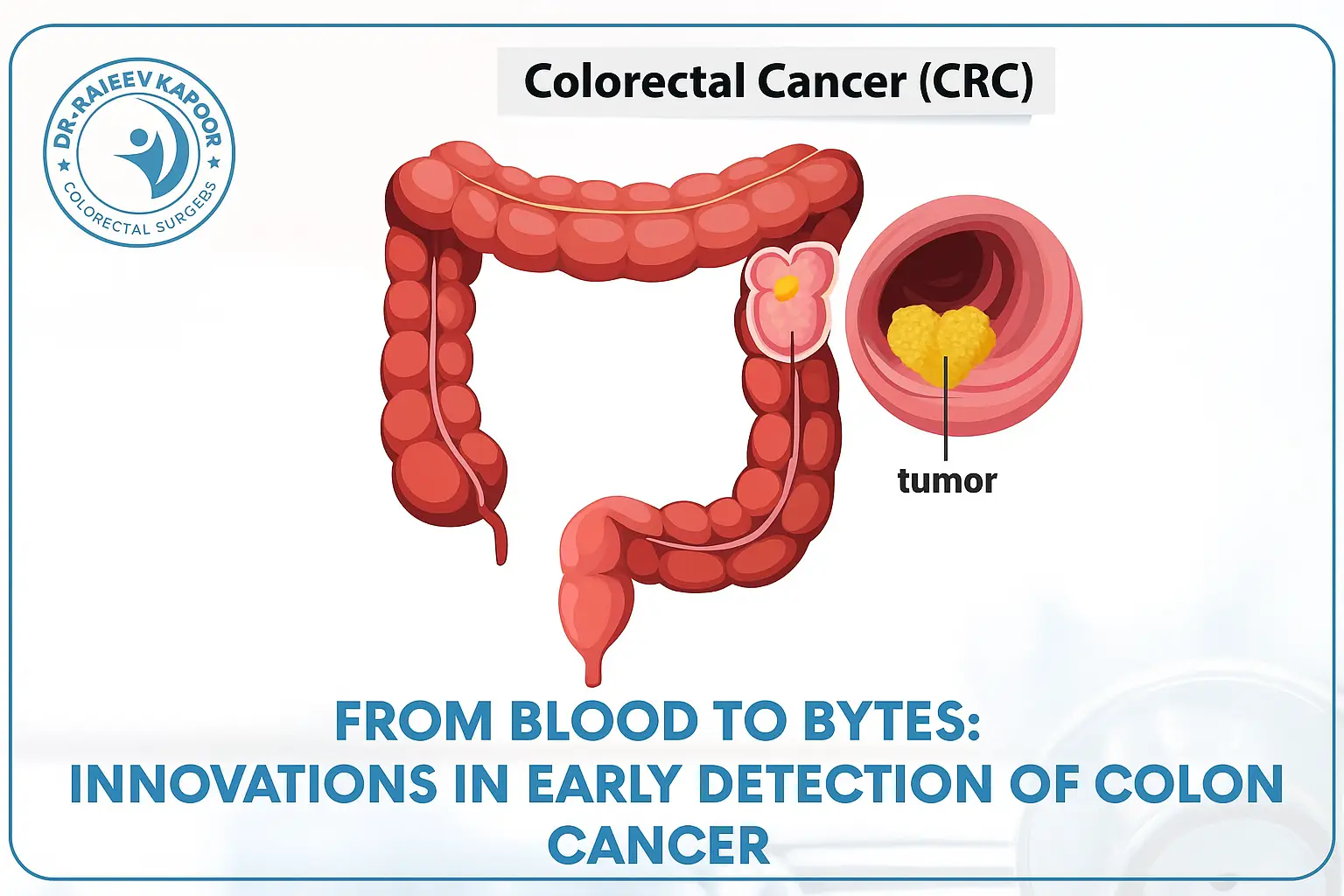
From Blood to Bytes: Innovations in Early Detection of Colon Cancer
Early detection is the most powerful tool in the fight against colon cancer (colorectal cancer). Traditionally, colonoscopy has been the gold standard for screening. But in 2025, medical science is taking bold strides with blood-based diagnostics, AI-powered imaging, and precision biomarkers. These innovations aim to make colon cancer detection earlier, easier, and more accurate, especially for patients who avoid invasive procedures. Liquid Biopsy: A Simple Blood Test One of the most exciting breakthroughs is the FDA-approved blood test “Shield” for average-risk individuals. Detects fragments of tumor DNA (circulating tumor DNA or ctDNA) in blood. Provides a non-invasive option for people unwilling or unable to undergo colonoscopy. Enhances compliance in population-based screening programs. This innovation could revolutionize colorectal cancer screening in India, where awareness and accessibility to colonoscopy remain limited. ctDNA for Treatment Decisions Beyond detection, ctDNA tests are now helping doctors personalize treatment: After surgery, ctDNA can indicate if microscopic cancer cells remain. Trials such as DYNAMIC-III show ctDNA can guide whether patients truly need chemotherapy after surgery, sparing many from unnecessary toxicity. In advanced disease, ctDNA also helps track resistance to therapy in real time. Artificial Intelligence (AI) in Colon Cancer AI is rapidly entering the field of colorectal cancer: Histopathology: New models like hybrid graph-transformers can classify colon cancer tissue with high accuracy. Colonoscopy assistance: AI tools flag polyps and lesions during endoscopy, reducing human error. Multimodal systems: Platforms like ColonScopeX combine blood signals, patient history, and explainable AI to predict colon cancer risk with high precision. These innovations promise earlier diagnosis, fewer missed lesions, and better patient outcomes. Next-Generation Technologies Nanotechnology: Indian researchers are exploring nanoparticle-based systems that deliver chemotherapy drugs directly to the colon, improving effectiveness and reducing side effects. Spatial molecular imaging: Provides deeper insights into tumor microenvironments, paving the way for highly targeted prevention and therapy. Wearable biosensors: Emerging research hints at stool/blood sensors that could track early biomarkers of colon cancer at home. Conclusion From blood tests to AI-powered diagnostics, the landscape of colon cancer detection is changing rapidly. These tools hold the potential to save countless lives by catching cancers earlier, when treatments are most effective. For patients seeking advanced care, Dr. Rajeev Kapoor, a renowned colorectal cancer surgeon in Mohali, India, offers cutting-edge screening and surgical expertise, ensuring access to world-class treatment close to home.