Necrotising fasciitis
Necrotising fasciitis is a rare but serious bacterial infection that affects the deeper layers of the skin and surrounding soft tissues, particularly the fascia (connective tissue surrounding muscles, nerves, and blood vessels). The infection can spread rapidly and may require urgent medical evaluation and treatment.
Although uncommon, necrotising fasciitis is considered a medical emergency because it can progress quickly and lead to severe complications if not treated promptly.
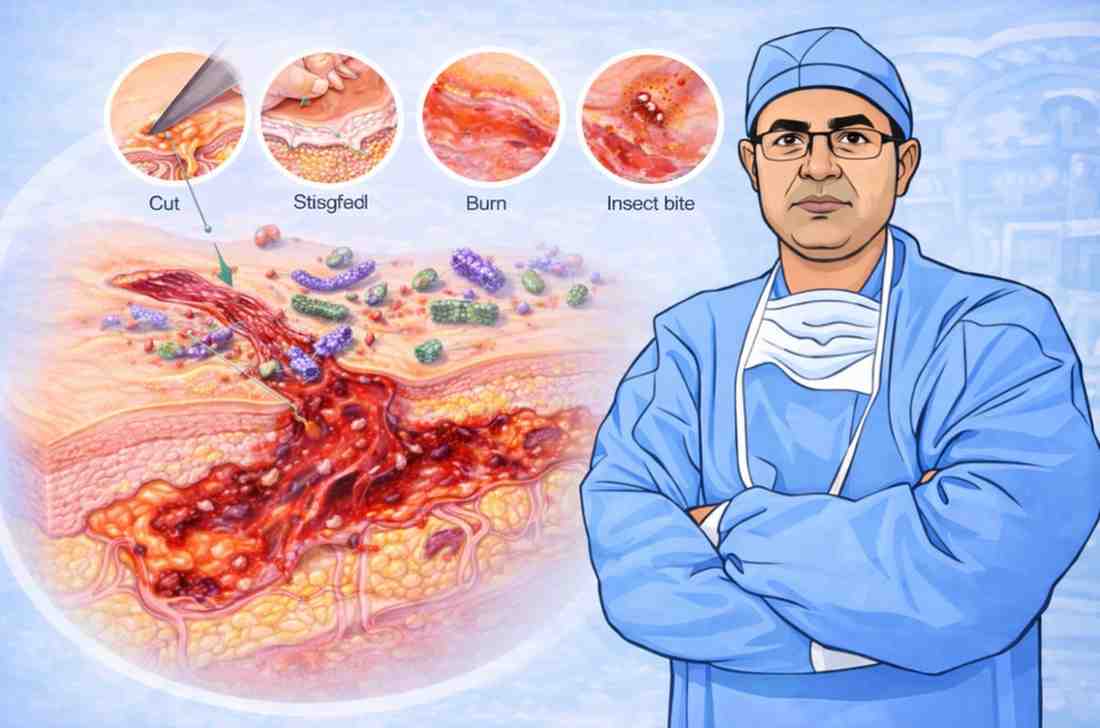
What is Necrotising Fasciitis?
Necrotising fasciitis is a severe infection that causes damage to the soft tissues beneath the skin. It occurs when bacteria enter the body through a break in the skin, such as a cut, surgical wound, burn, insect bite, or injury.
Once inside the body, the bacteria may spread along the fascia, causing inflammation, tissue damage, and destruction of affected tissues.
Causes
Necrotising fasciitis is most commonly caused by bacterial infections. Several types of bacteria may be involved, including:
- Group A Streptococcus bacteria
- Staphylococcus bacteria
- Clostridium species
- Mixed bacterial infections involving multiple organisms
In some cases, the infection may occur after trauma, surgery, or skin infections.
Symptoms
Symptoms may develop rapidly and can worsen over a short period. Common symptoms may include:
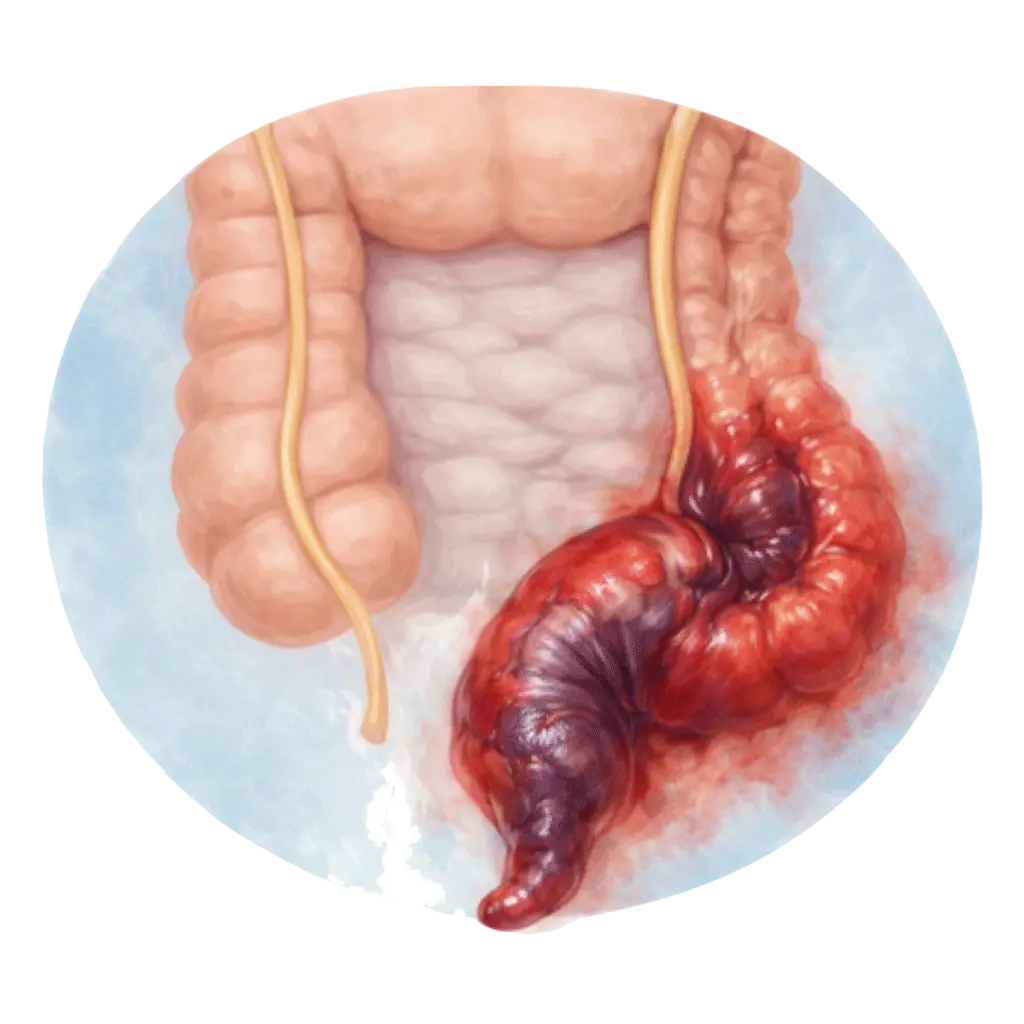
Severe pain that may appear disproportionate to the visible skin changes
Swelling and redness of the affected area

Fever and chills
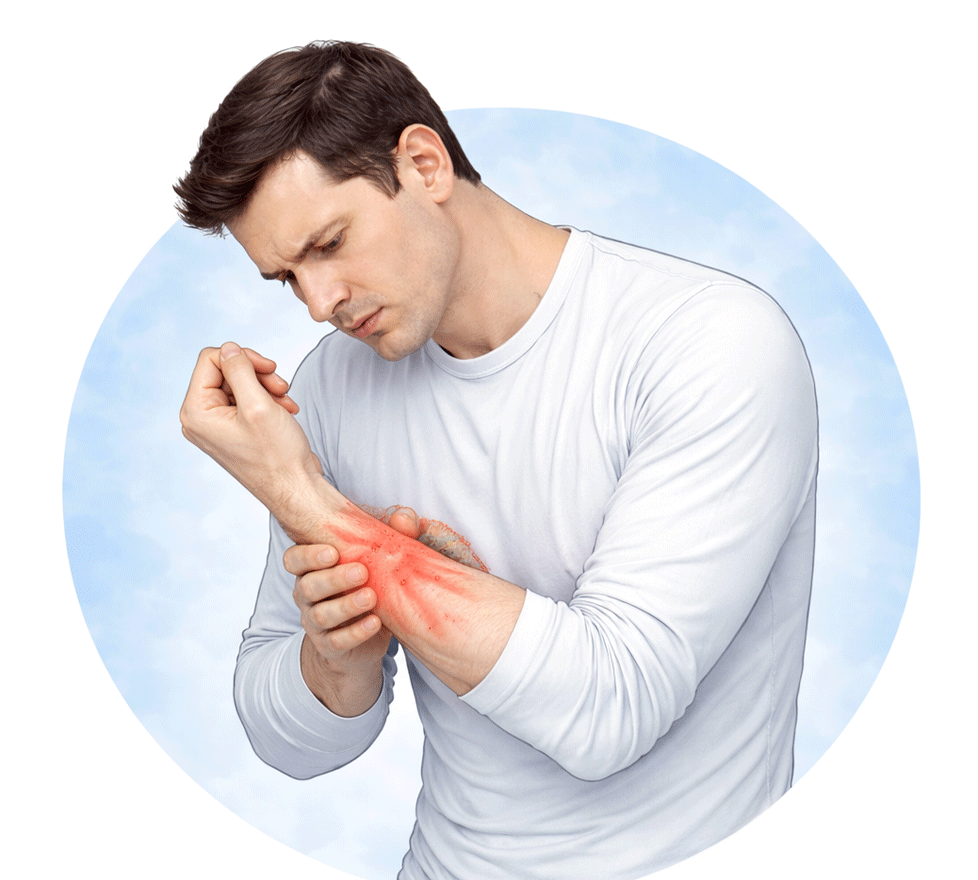
Skin warmth and tenderness
As the infection progresses, the skin may show signs of tissue damage or necrosis.
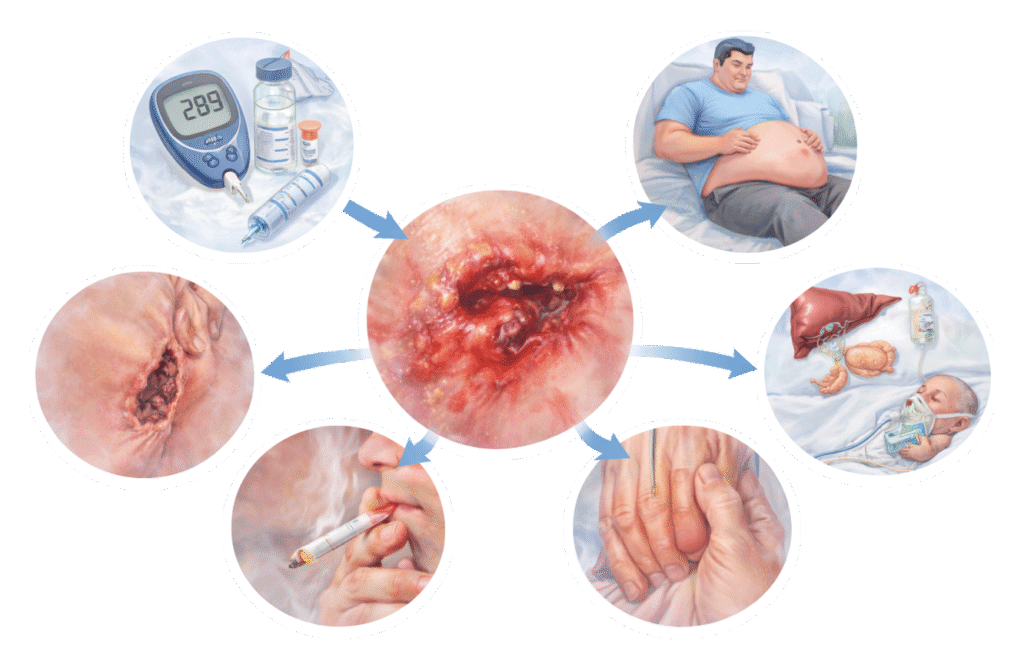
Risk Factors
Certain conditions may increase the risk of developing necrotising fasciitis, such as:
- Diabetes mellitus
- Weakened immune system
- Chronic liver or kidney disease
- Obesity
- Recent surgery or injury
- Chronic skin wounds
However, the condition can occasionally occur in otherwise healthy individuals.
Diagnosis
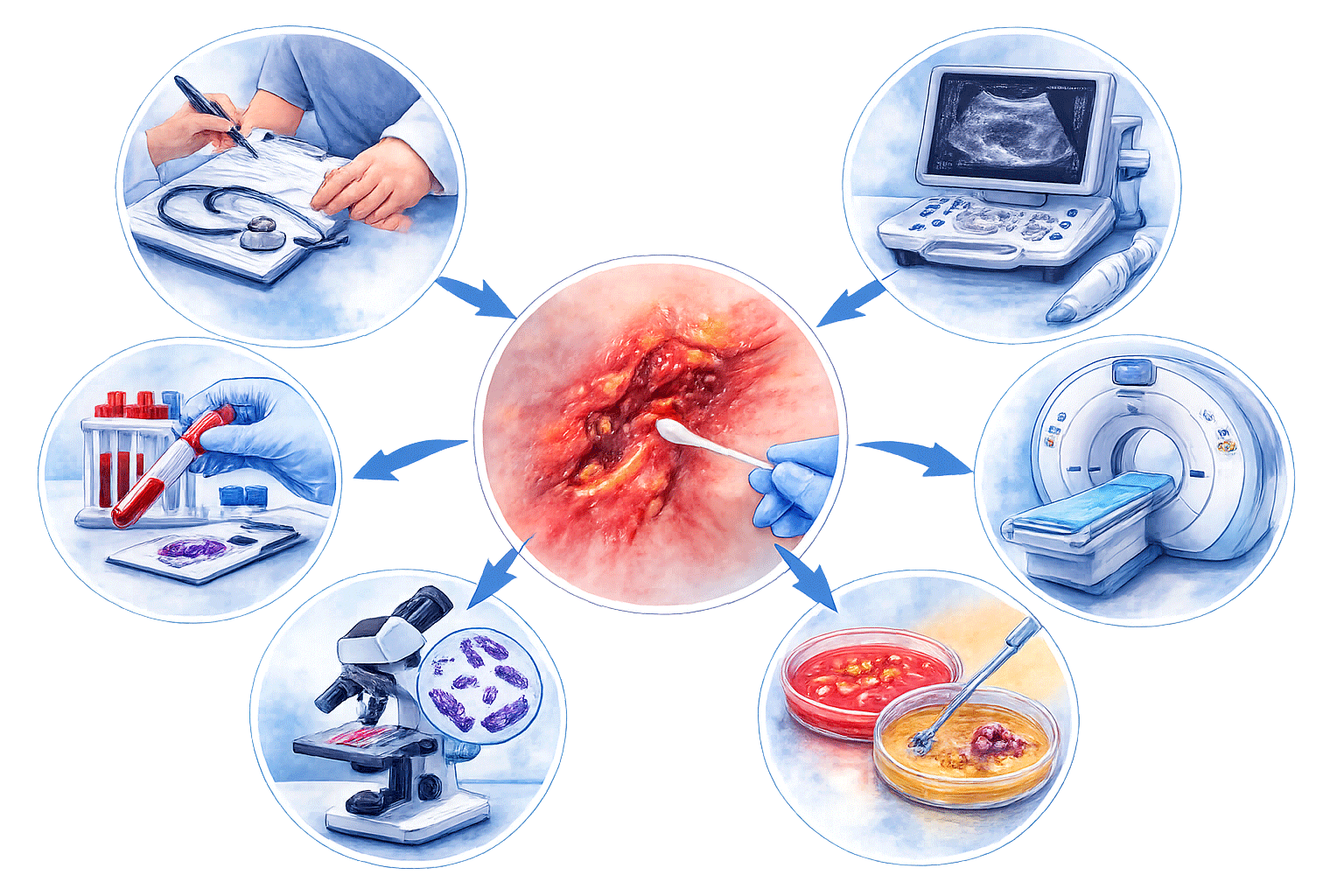
Early diagnosis is important for appropriate management. Healthcare professionals may evaluate:
- Medical history and symptoms
- Physical examination of the affected area
- Blood tests
- Imaging tests such as ultrasound, CT scan, or MRI
- Tissue or fluid samples to identify the bacteria
These investigations help confirm the diagnosis and guide treatment.
Treatment
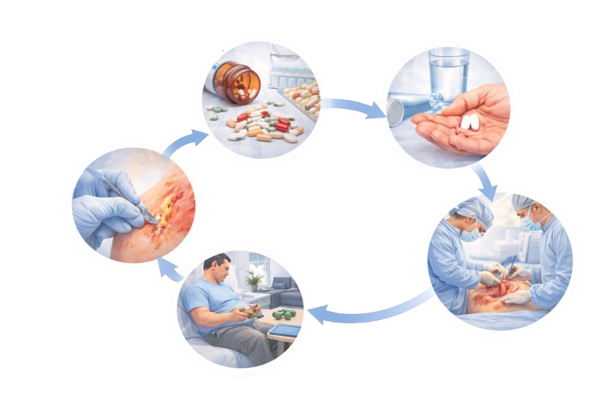
Necrotising fasciitis requires urgent medical care. Treatment may include:
- Hospital admission
- Intravenous antibiotics to control infection
- Surgical removal of infected or dead tissue (debridement)
- Supportive care in a hospital setting
In severe cases, multiple procedures may be required to control the spread of infection.
Possible Complications
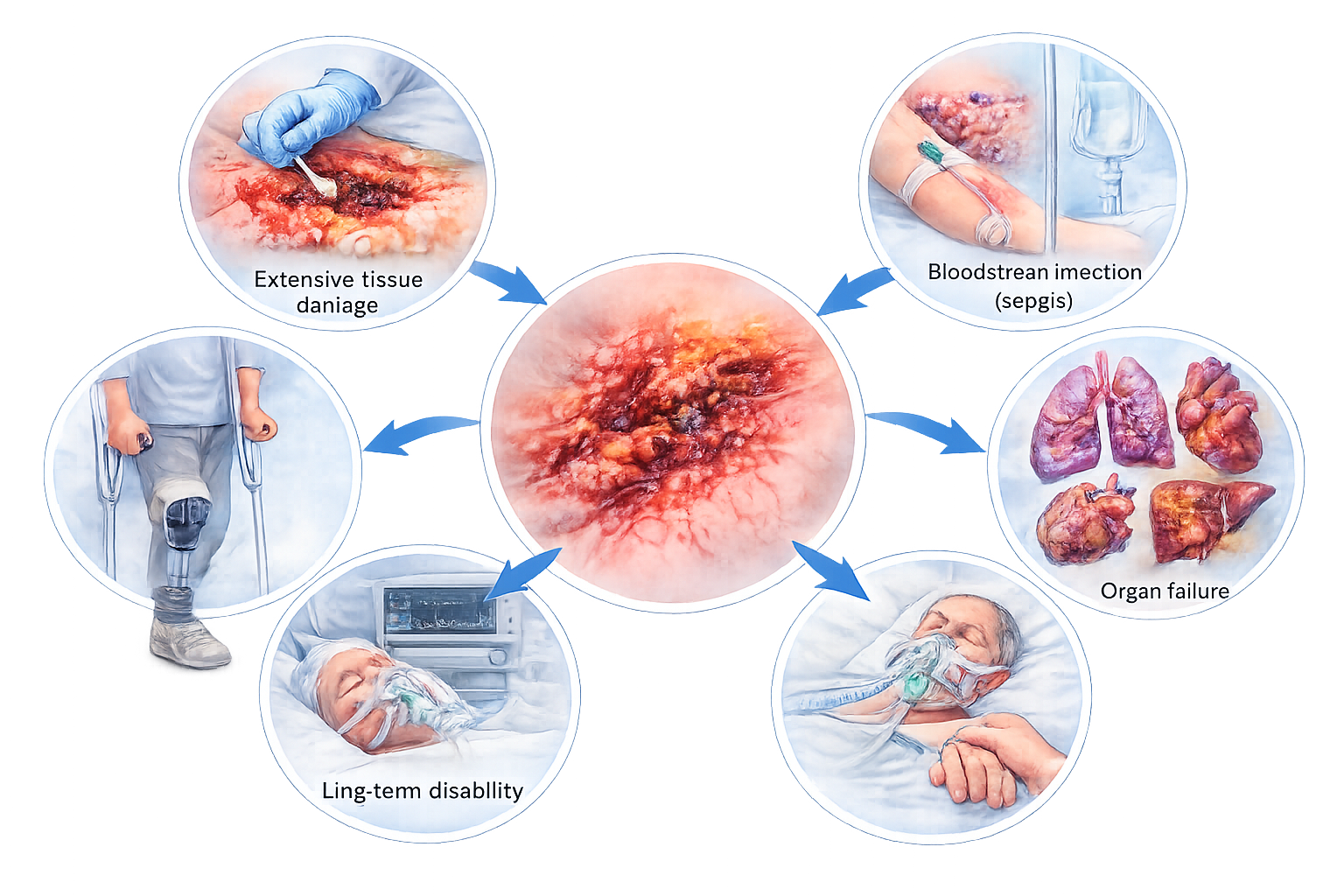
If not treated promptly, necrotising fasciitis may lead to serious complications such as:
- Extensive tissue damage
- Bloodstream infection (sepsis)
- Organ failure
- Long-term disability
- In rare cases, life-threatening outcomes
Early medical intervention can help improve outcomes.
Prevention
Although it may not always be preventable, certain precautions may reduce the risk:
- Proper wound care and cleaning of cuts or injuries
- Seeking medical attention for infected wounds
- Maintaining good hygiene
- Managing chronic medical conditions such as diabetes

When to Seek Medical Attention
Immediate medical attention may be necessary if a person experiences:
- Severe pain near a wound or injury
- Rapidly spreading redness or swelling
- Fever with worsening skin infection
- Skin discoloration or blistering
Early evaluation is important to prevent complications.
About the Author of This Information
Dr. Rajeev Kapoor is a practicing surgeon based in Mohali, Punjab. He provides clinical services in the field of gastrointestinal, colorectal, and general surgery. This website is intended for informational and educational purposes only.
Disclaimer
The information provided on this page is for general educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Treatment decisions should be made after consultation with a qualified medical professional, based on individual clinical evaluation.

