Early Warning Signs of Colon Cancer You Shouldn’t Ignore
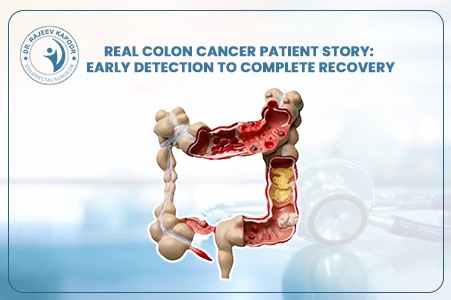
Introduction Colon cancer, also known as colorectal cancer, is among the top five cancers affecting men and women in India. Yet, most patients are diagnosed only when the disease has already advanced. According to Dr. Rajeev Kapoor, a renowned gastrointestinal and cancer surgeon in Chandigarh, “Early detection is the key to saving lives. Awareness of the initial warning signs can make all the difference.” 1️⃣ Change in Bowel Habits One of the earliest indicators of colon cancer is a persistent change in bowel movements—such as diarrhea, constipation, or a feeling that the bowel does not empty completely. If such symptoms last more than two weeks, they should not be ignored. 💡 Tip from Dr. Kapoor: “If your bowel habits have changed and do not respond to routine diet adjustments, consult your doctor for evaluation.” 2️⃣ Blood in Stool or Rectal Bleeding The appearance of bright red or dark blood in stool may signal bleeding from the lower intestine. Though hemorrhoids are a common cause, hidden bleeding could also indicate colorectal cancer. Periodic screening can detect such bleeding early, even before visible symptoms appear. 3️⃣ Unexplained Weight Loss and Fatigue Unintentional weight loss, fatigue, or persistent weakness could point to a deeper issue. Cancer cells consume more energy, while slow internal bleeding can lead to iron-deficiency anemia, which often manifests as chronic tiredness. 4️⃣ Abdominal Pain and Bloating Patients may experience cramping, gas, or discomfort in the lower abdomen. These symptoms can be mistaken for IBS (Irritable Bowel Syndrome) but, when persistent, require a colonoscopy to rule out malignancy. 5️⃣ Family History and Genetic Risk Individuals with a family history of colon or rectal cancer—or conditions such as Lynch syndrome or familial adenomatous polyposis (FAP)—have a significantly higher risk. Dr. Kapoor recommends screening colonoscopy starting at age 45 or even earlier for those with genetic predispositions. Why Early Detection Matters When colon cancer is caught early, the survival rate can exceed 90 %. Screening methods like colonoscopy, stool occult blood tests, and CT colonography can identify precancerous polyps that can be removed before they turn cancerous. 🩺 “Every colon cancer begins as a small, silent polyp. Detecting it before it turns malignant can save a life,” emphasizes Dr. Kapoor. Prevention and Lifestyle Tips Eat a fiber-rich diet (fruits, vegetables, whole grains) Limit red and processed meat Maintain a healthy weight and regular exercise routine Avoid smoking and excess alcohol Schedule periodic screenings after 45 (or earlier if at risk) Conclusion Colon cancer is preventable, treatable, and—even in many cases—curable when detected early. Awareness of these warning signs and timely medical evaluation can dramatically improve outcomes. If you or a loved one experience any of these symptoms, don’t delay.