Surgical Strategies To Address Intestinal Obstruction
Intestinal obstruction is a serious medical condition where there is a partial or complete blockage of the normal flow of digestive contents through the intestines. When conservative measures like nasogastric tube decompression and medication fail to relieve the obstruction, surgical intervention becomes necessary.
Indications For Surgery
Surgical intervention is considered when:-
- Conservative Measures Fail: Initial attempts to relieve the obstruction using non-surgical methods like placing a nasogastric tube and administering medications do not work.
- Strangulation: When the blood supply to a segment of the intestine is compromised due to the obstruction, immediate surgery is required to prevent tissue death (Gangrene).
- Complete Obstruction: In cases of complete bowel obstruction where no gas or stool can pass through, surgery is often necessary.
Surgical Options
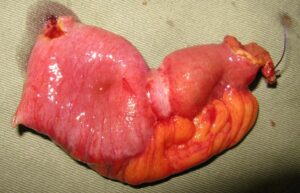
Bowel Resection And Anastomosis
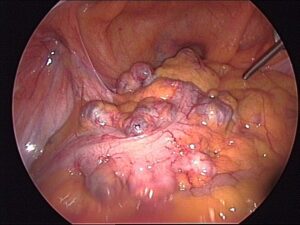
- Indications: This is commonly used when there’s a mechanical obstruction due to conditions like tumors, strictures, or volvulus.
- Procedure: The surgeon removes the affected or obstructed segment of the intestine and then joins the healthy ends together, creating an anastomosis. This procedure allows for the restoration of normal bowel continuity.
- Considerations: The length of the resected segment and the health of the remaining bowel are essential factors in determining the type of anastomosis and whether a temporary or permanent stoma (opening on the abdominal wall) is needed.
Bowel Bypass
- Indications: This approach is used when resection and anastomosis are not feasible due to the patient’s condition or the site of obstruction.
- Procedure: The surgeon creates a bypass around the obstructed area using healthy segments of the intestine. This allows digestive contents to bypass the blocked section and continue through the bowel.
- Considerations: Bowel bypass is typically a palliative procedure and may require further surgeries or interventions.
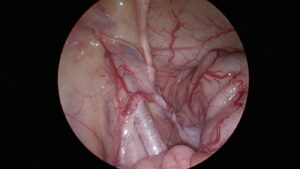
Adhesiolysis
- Indications: Adhesions, which are bands of scar tissue, can cause mechanical obstructions. Adhesiolysis involves cutting or separating these adhesions to free the bowel.
- Procedure: The surgeon carefully dissects and removes the adhesions that are causing the obstruction.
- Considerations: Adhesiolysis is often performed using minimally invasive laparoscopic techniques when possible.
Strictureplasty
- Indications: In cases of strictures, which are narrowed segments of the intestine, strictureplasty can be performed.
- Procedure: The surgeon makes longitudinal incisions in the strictured segment to widen it without removing any bowel.
- Considerations: This approach is used when preserving as much functional bowel as possible is essential.
Ostomy Creation
- Indications: In some cases, particularly if the bowel is severely damaged or infection is present, a temporary or permanent ostomy may be created.
- Procedure: An ostomy involves bringing a portion of the bowel to the surface of the abdomen to allow for the elimination of stool or gas through a stoma.
- Considerations: Temporary ostomies can often be reversed in a later surgery, while permanent ostomies are permanent.
Postoperative Care
After Intestinal obstruction surgery, patients are closely monitored for complications, including infection, wound healing, and ileus (temporary paralysis of the bowel). Nutritional support and gradual reintroduction of food are also crucial aspects of postoperative care.
Conclusion
Surgical management of Intestinal obstruction depends on the underlying cause, the location and severity of the obstruction, and the overall health of the patient. Surgeons must carefully evaluate each case to determine the most appropriate surgical approach, whether it involves resection, bypass, adhesiolysis, strictureplasty, or ostomy creation. Early intervention and effective surgical treatment are vital to improve patient outcomes and prevent complications associated with this serious condition.
Also Read:
Surgical Options For Anal Or Fecal Incontinence
The Rising Incidence of Colorectal Cancer In India
Treatment of Fecal Incontinence In Women of Childbearing Age