Appendicitis — Symptoms, Diagnosis & Surgery
A practical guide to understanding appendicitis — what causes it, how it is diagnosed, and what surgery involves.

What Is Appendicitis?
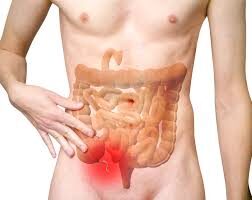
Appendicitis is an inflammation of the appendix — a small, finger-shaped pouch attached to the beginning of your large bowel (the caecum), in the lower right side of your abdomen. It is one of the most common surgical emergencies worldwide.
When the opening of the appendix gets blocked — usually by hardened stool (a faecolith), swollen lymph tissue, or rarely a tumour — bacteria multiply inside, the wall becomes inflamed and swollen, and pressure builds. If not treated, the appendix can perforate (burst), spilling infected material into the abdominal cavity.
Appendicitis can occur at any age but is most common between the ages of 10 and 30. It affects both men and women. The lifetime risk of developing appendicitis is approximately 7–8%.
What Causes Appendicitis?
Appendicitis develops when the opening of the appendix becomes blocked, allowing bacteria to multiply inside and trigger infection. Several things can cause this blockage.
Hardened Stool (Faecolith)
The most common cause. A small, calcified piece of stool lodges at the base of the appendix, blocking drainage and allowing bacteria to accumulate inside.
Swollen Lymph Tissue
After a viral illness, lymphoid tissue inside the appendix wall can swell (lymphoid hyperplasia), narrowing the opening. This is especially common in children and young adults.
Diet & Lifestyle Factors
A low-fibre diet is associated with a higher risk of appendicitis. Fibre keeps stool soft and reduces the chance of faecolith formation. Severe physical stress may also reduce blood flow to the gut and contribute.
Less Common Causes
Rarely, a tumour, intestinal parasite, or mucus plug can obstruct the appendix. A family history of appendicitis may also increase your risk, though the exact mechanism is not fully understood.
Symptoms — How Does Appendicitis Feel?
The classic pattern is pain that starts around the navel and then moves to the lower right side of the abdomen — but not everyone follows this textbook pattern.
Abdominal Pain
Usually begins as a dull ache around the belly button, then shifts to the right lower abdomen (right iliac fossa) over 6–24 hours. The pain gets steadily worse and is aggravated by movement, coughing, or pressing on the area.
Loss of Appetite & Nausea
Most patients lose their appetite (anorexia). Nausea and vomiting often follow the onset of pain — typically after the pain starts, not before.
Fever
A low-grade fever (37.5–38.5 °C) is common. A high fever (>39 °C) may suggest that the appendix has perforated or an abscess has formed.
Other Signs
Tenderness when pressing the right lower abdomen, pain on releasing pressure (rebound tenderness), inability to pass gas, and sometimes loose stools or urinary frequency (if the appendix lies near the bladder).
- ⚠ Severe or worsening abdominal pain, especially in the right lower side
- ⚠ Pain that suddenly becomes much worse — this may mean the appendix has burst
- ⚠ Fever with abdominal pain and vomiting
- ⚠ Inability to eat or drink anything due to pain and nausea
- ⚠ Abdominal rigidity — the belly feels hard and board-like
How Is Appendicitis Diagnosed?
Diagnosis is based on your symptoms, a physical examination by the surgeon, blood tests, and usually an imaging scan. In many cases, an experienced surgeon can diagnose appendicitis at the bedside.
Blood Tests
A raised white blood cell count (WBC) and elevated CRP (C-reactive protein) support the diagnosis. These are not specific to appendicitis but indicate inflammation or infection.
Ultrasound
Often the first imaging test — especially in children and young women. It can show a swollen, non-compressible appendix. No radiation exposure.
CT Scan
The most accurate imaging test for appendicitis in adults. Shows the inflamed appendix, any perforation, abscess, or alternative diagnosis. Used when ultrasound is inconclusive or when complications are suspected.
An experienced surgeon can often diagnose appendicitis through a focused physical examination. These are the key signs assessed at the bedside:
- McBurney’s Point Tenderness — Maximum tenderness at a specific point one-third of the way from the right hip bone to the navel. A classic finding in acute appendicitis.
- Blumberg’s Sign (Rebound Tenderness) — Pain is worse when the examining hand is quickly released than when pressure is applied. Suggests peritoneal irritation.
- Rovsing’s Sign — Pressing the left side of the abdomen produces pain on the right. Indicates referred peritoneal irritation from the inflamed appendix.
- Dunphy’s Sign — A cough or sudden movement sharply increases the pain. Another marker of peritoneal irritation.
- Psoas Sign — Pain on extending the right hip while lying on the left side, suggesting the appendix lies close to the psoas muscle (retrocaecal position).
- Obturator Sign — Pain on internal rotation of the right hip, suggesting a pelvic appendix lying near the obturator muscle.
No single sign confirms the diagnosis on its own. Your surgeon interprets these findings alongside your history, blood tests, and imaging to reach a clinical decision.
Several other conditions can cause similar symptoms. Your surgeon considers these during the assessment:
- Mesenteric lymphadenitis — swollen lymph nodes in the abdomen (common in children after a viral illness)
- Ovarian cyst (torsion or rupture) — in women of reproductive age
- Ectopic pregnancy — must be excluded in all women of childbearing age with lower abdominal pain
- Right ureteric colic (kidney stone)
- Meckel’s diverticulitis
- Crohn’s disease affecting the terminal ileum — read more on our IBD page
- Caecal diverticulitis or a caecal/appendiceal tumour
If there is diagnostic uncertainty, a CT scan or diagnostic laparoscopy (keyhole camera look inside the abdomen) may be performed.
Types of Appendicitis
Uncomplicated (Simple) Appendicitis
The appendix is inflamed but has not perforated. This is the most common presentation. Early surgery gives excellent results with a short hospital stay.
Complicated Appendicitis — Perforation
The appendix has burst (perforated). Infected material leaks into the abdomen, causing peritonitis (widespread infection of the abdominal lining). This requires urgent surgery and a longer course of antibiotics.
Appendicular Abscess / Lump
Sometimes, a perforated appendix gets walled off by the body’s own tissues, forming a localised collection of pus (abscess) or a firm mass (appendicular lump). Treatment may involve antibiotics and drainage first, with surgery planned later (an “interval appendicectomy”).
Chronic / Recurrent Appendicitis
A less recognised form where the appendix becomes intermittently inflamed over weeks or months, causing recurring episodes of right lower abdominal pain that settle on their own. Each episode carries the risk of progressing to perforation. Surgical removal of the appendix is the definitive treatment.
Why timing matters: Uncomplicated appendicitis can progress to perforation within 24–72 hours of symptom onset. This is why abdominal pain that is worsening should never be ignored — early assessment and timely surgery prevent complications.
The Operation — Appendicectomy
The standard treatment for appendicitis is surgical removal of the appendix — an operation called an appendicectomy (also spelled appendectomy). It can be performed laparoscopically (keyhole) or as an open operation.
Laparoscopic Appendicectomy
Done through 3 small incisions (5–10 mm each) using a camera and specialised instruments. The appendix is identified, its blood supply secured, and the base divided and removed. This is the preferred approach in most cases — less pain, faster recovery, smaller scars, lower wound infection rate.
Open Appendicectomy
Done through a small incision in the right lower abdomen (McBurney’s or Lanz incision). Still widely used when laparoscopic equipment is not available, when the appendix has perforated with extensive contamination, or when the surgeon encounters dense adhesions.
In carefully selected patients with early, uncomplicated appendicitis and no perforation, a short course of intravenous antibiotics can settle the inflammation without immediate surgery. Several international trials have shown this is feasible in the short term.
However, there are important limitations:
- Around 1 in 3 patients treated with antibiotics alone will develop appendicitis again within a year and eventually require surgery
- A small number of patients thought to have uncomplicated appendicitis are found to have a faecolith or early perforation — these do not respond reliably to antibiotics
- Antibiotic treatment requires close monitoring in hospital and is not suitable for everyone
Surgery remains the standard treatment because it eliminates the risk of recurrence and removes any uncertainty about what is inside the appendix.
Your surgeon will discuss which approach is appropriate for your individual situation.
The operation is performed under general anaesthesia. The key steps are:
- Three small ports (cuts) are placed — one at the navel, and one or two on the lower abdomen
- Carbon dioxide gas is used to gently inflate the abdomen, creating space for the camera and instruments
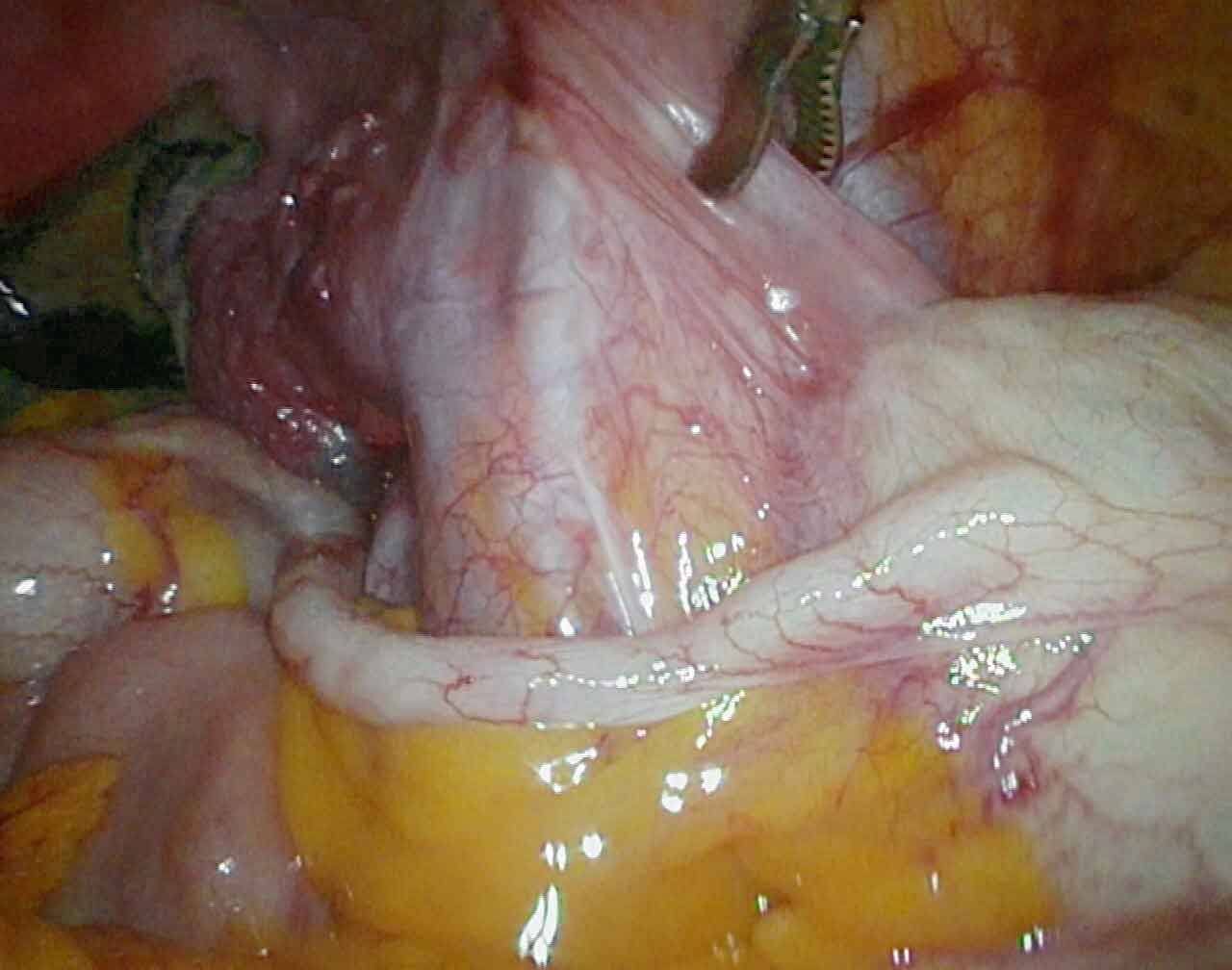
- The surgeon identifies the appendix and carefully separates it from surrounding tissues
- The blood supply to the appendix (the mesoappendix) is sealed and divided
- The base of the appendix is secured with clips or a loop (endoloop) and the appendix is cut free
- The appendix is placed in a bag and removed through one of the port sites
- The abdomen is washed if there is any pus or contamination
The operation typically takes 30–60 minutes for uncomplicated cases. If the appendix has perforated or there is an abscess, the operation may take longer and include a thorough washout of the abdominal cavity.
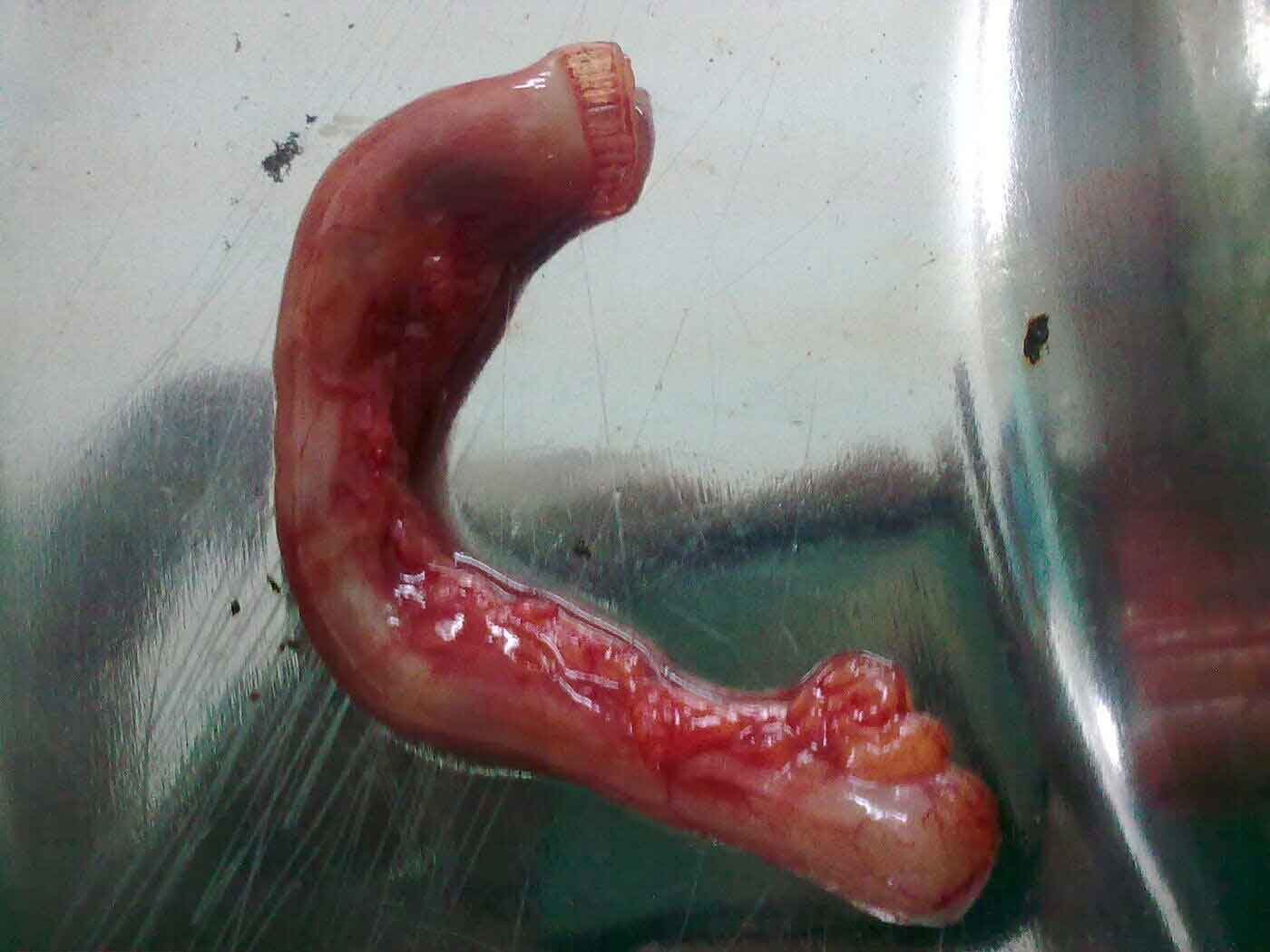
In most cases, the base of the appendix (the point where it joins the caecum) is healthy enough to be closed safely with a loop ligature or clip. However, in severe or delayed presentations, gangrene and necrosis can extend all the way to the base, making standard closure unsafe — a loop placed on dead tissue will cut through and leak.
In these situations, the surgeon uses an Endo-GIA linear stapler to divide and seal the bowel across a small rim of healthy caecal tissue, just beyond the gangrenous area. This creates a clean, secure staple line on tissue that is not diseased. A small portion of the caecal wall is included in the stapled segment and removed with the appendix — this is entirely safe and does not affect how the remaining bowel functions.
Published surgical data show a stump leak rate of 0% with this technique in experienced hands, and mean hospital stay in these more complex cases is approximately 4–5 days. Recovery is typically uneventful. Most patients are on a normal diet and walking within 24–48 hours of surgery.
The decision to use a stapler is made intraoperatively by the surgeon based on the condition of the tissue. It does not change your long-term outcome — the caecum heals completely and bowel function is unaffected.
This is one of the most common questions families ask when a diagnosis is made late at night. The honest answer is: it depends on the severity of the case, not the time on the clock.
For uncomplicated appendicitis — where the appendix is inflamed but not yet perforated, and the patient is stable — the medical evidence is reassuring. Large studies involving tens of thousands of patients have consistently shown that a delay of up to 18 hours from the time of diagnosis does not increase the risk of perforation, complications, or a longer hospital stay. In practice, this means a patient diagnosed at midnight can safely be operated on first thing in the morning, after a proper night's rest for the surgical team, full preparation, and optimal theatre conditions.
For complicated appendicitis — where there is already perforation, generalised peritonitis, an abscess, or the patient is deteriorating — waiting is not appropriate. These patients need surgery as soon as they are adequately resuscitated, regardless of the hour.
The decision is always made by the surgeon after directly assessing the patient — not by a fixed rule about time. What matters most is a careful, unhurried operation by a prepared team, not one performed under pressure at 3 in the morning.
What the Pathology Report Can Reveal
Every appendix removed at surgery — regardless of whether it looks straightforward — is sent to the pathology laboratory for microscopic examination. This is not a formality. In approximately 1 in 100 cases, the pathologist identifies an unexpected tumour inside the appendix that was clinically invisible during the operation.
The appendix can harbour several distinct tumour types, each with different behaviour and management requirements:
- Neuroendocrine Tumours (NETs / Carcinoid) — the most common appendiceal tumour, accounting for up to 80% of cases. Over half are found incidentally on pathology. Tumours smaller than 2 cm are cured by appendicectomy alone. Tumours 2 cm or larger carry a risk of lymph node spread and require a right hemicolectomy (removal of the right colon) as a second operation.
- Low-Grade Appendiceal Mucinous Neoplasm (LAMN) — a mucus-producing tumour that, if the appendix has perforated, can seed the abdominal cavity and cause a serious condition called pseudomyxoma peritonei. Early detection through pathology allows planning before this complication develops.
- Goblet Cell Carcinoma & Adenocarcinoma — rarer and more aggressive. These almost always require right hemicolectomy and oncological follow-up by a colorectal and cancer surgery team.
Because more than half of all appendiceal tumours produce no symptoms and are invisible to the naked eye at surgery, routine histopathological examination of every appendix specimen is essential. Skipping pathology is not an option — it risks missing a diagnosis that is entirely treatable when caught early.
If a tumour is found on your pathology report, your surgeon will review the findings with you and discuss whether any further surgery or investigation is needed.
Appendicular Lump & Interval Appendicectomy
When appendicitis has been present for several days, the body sometimes walls off the infection, forming an appendicular lump or abscess. In these cases, immediate surgery can be technically difficult and risky.
Conservative Treatment First
- Hospital admission, intravenous antibiotics, pain relief, and close monitoring
- If an abscess is identified on CT or ultrasound, it may be drained using a needle or small tube placed through the skin (percutaneous drainage)
- Most patients improve within 3–5 days and can be discharged on oral antibiotics
Interval Appendicectomy
Once the inflammation has completely settled (usually 6–8 weeks later), the surgeon will recommend an interval appendicectomy — a planned, elective operation to remove the appendix. This is done because:
- There is a significant risk of the appendicitis coming back (recurrence rate ~20–30%)
- In patients over 40, a CT or colonoscopy is recommended before the interval surgery to rule out an underlying appendiceal or caecal tumour
Recovery After Appendicectomy
Hospital Stay
Uncomplicated laparoscopic appendicectomy: most patients go home within 24–48 hours. Complicated cases (perforation, abscess): 3–7 days depending on response to antibiotics.
Diet & Activity
Start with clear liquids, progress to a normal diet as tolerated. Light walking from day one. Avoid heavy lifting for 2–3 weeks (laparoscopic) or 4–6 weeks (open).
Return to Work
Desk job: 1–2 weeks. Physical or manual work: 3–4 weeks. Your surgeon will advise based on your individual recovery.
For detailed guidance on wound care, diet, exercise, and warning signs after surgery, visit our Recovery After Surgery page.
Possible Complications
Appendicectomy is a safe and common operation, but like any surgery it carries some risks.
Wound Infection
The most common complication, especially after open surgery or perforated appendicitis. Signs: redness, swelling, pus, or increasing pain at the wound site. Usually treated with antibiotics and wound care.
Intra-Abdominal Abscess
A collection of pus can form inside the abdomen after surgery, particularly if the appendix was perforated. Symptoms: persistent fever, abdominal pain, loss of appetite days after surgery. May need drainage (CT-guided) or antibiotics.
Bleeding
Uncommon. Usually controlled during surgery. Rarely requires a return to the operating theatre.
Injury to Surrounding Structures
Rare. The caecum, small bowel, or blood vessels near the appendix can occasionally be injured, especially in complicated or re-do surgery.
Stump Appendicitis
Very rare. If a small remnant of the appendix is left behind, it can become inflamed in the future. More common after difficult operations where the base of the appendix was severely inflamed.
Incidental Findings on Pathology
The removed appendix is always sent for examination under a microscope. Occasionally, the pathologist may find an unexpected tumour (such as a carcinoid or mucinous neoplasm). If this happens, your surgeon will discuss whether any further treatment or follow-up is needed. Read more on our appendiceal cancer page.
Frequently Asked Questions
Abdominal Pain Should Not Be Ignored
If you or a family member has sudden or worsening abdominal pain, timely assessment is important. Understanding your condition is the first step towards the right treatment.
Contact for Further InformationRelated Pages
For appointments or enquiries: Contact page | drrajeevkapoor.com