Your Journey from Symptom to Recovery
Understanding each step helps reduce anxiety and lets you prepare. Most patients move from first consultation to discharge within 2–3 days.
Preparing for Cholecystectomy
Getting to surgery safely involves a systematic pre-operative process. Here is what to expect from diagnosis to the day of the operation.
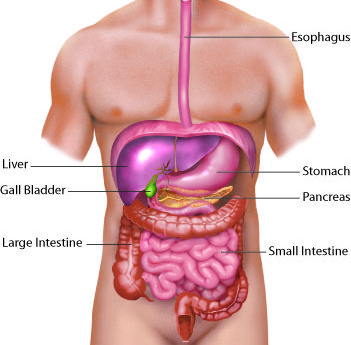
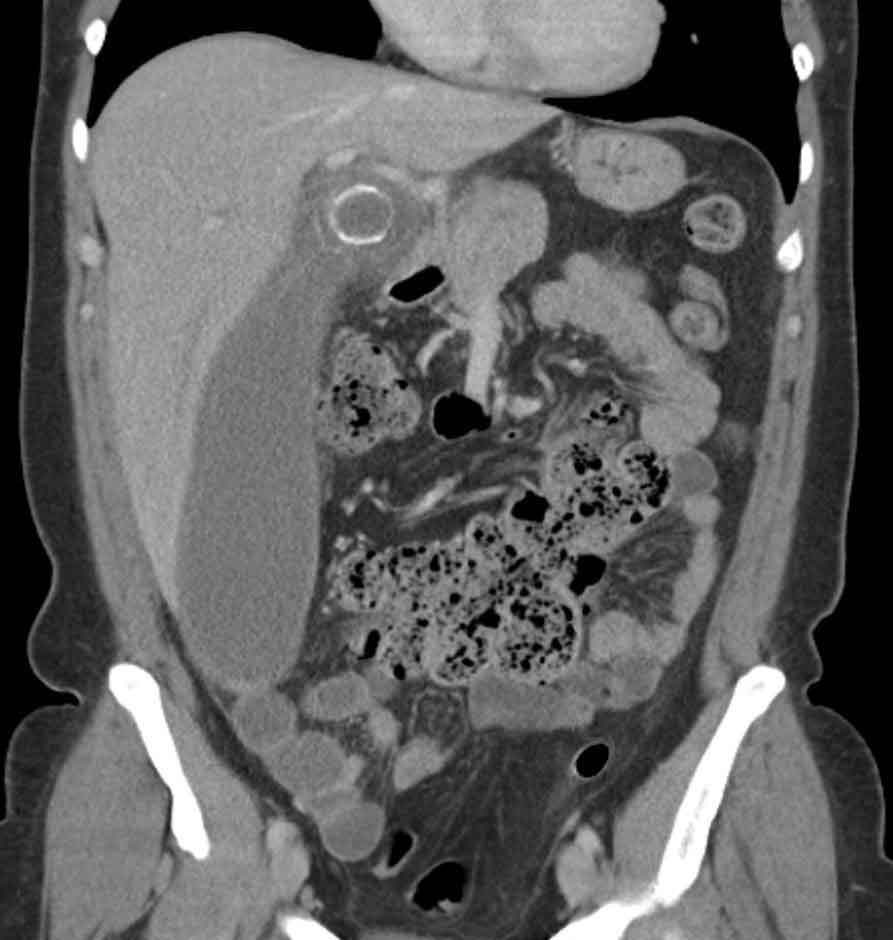
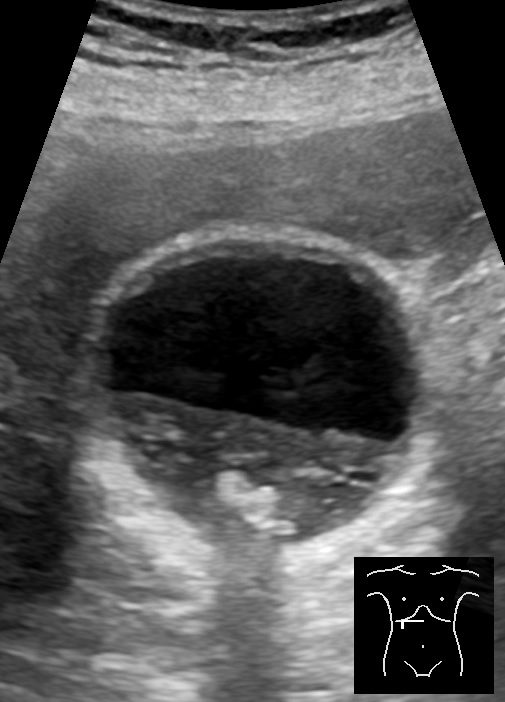
Confirming the Diagnosis
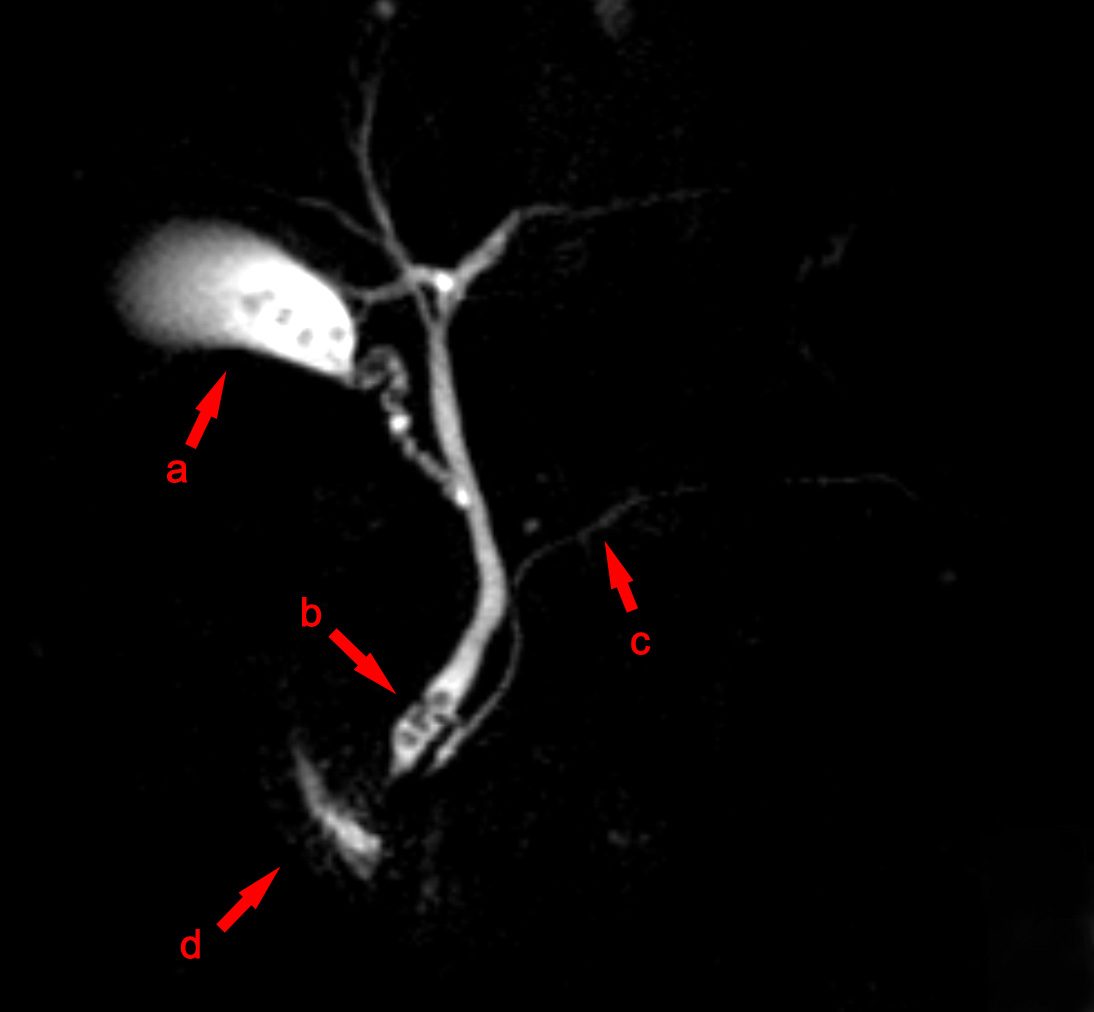
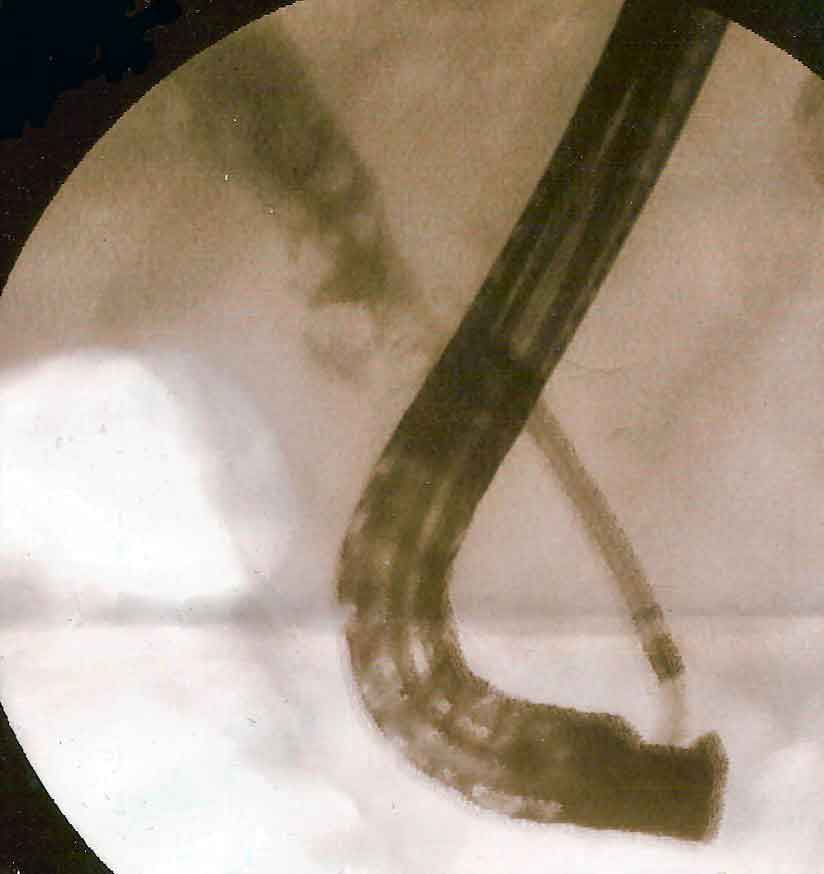
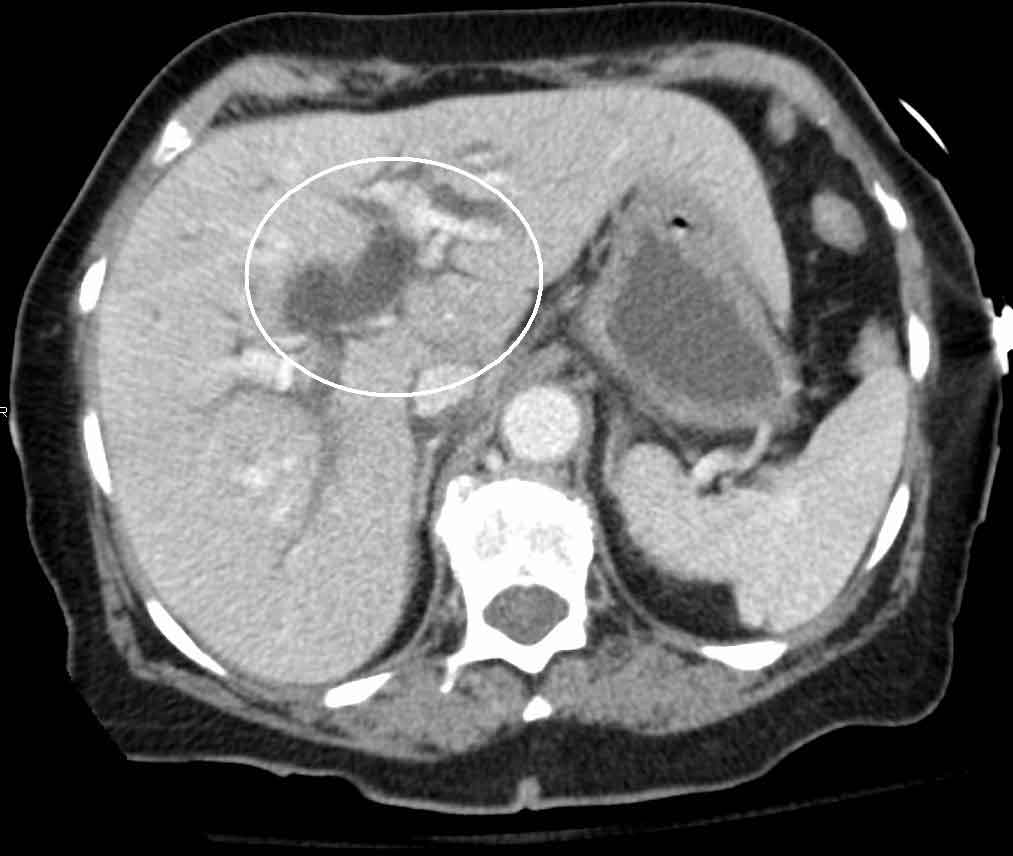
An ultrasound abdomen is the starting point for most patients. If bile duct involvement is suspected, MRCP is arranged. Blood tests — liver function, full blood count, kidney function, blood sugar, and clotting — are ordered. All imaging and reports are reviewed together before any decision is made.
Pre-Anaesthesia Check (PAC)
A formal assessment by the anaesthesia team. This includes a review of your full medical history, current medications, allergies, previous anaesthesia reactions, and fitness for surgery. An ECG and chest X-ray are ordered for patients over 40 or those with heart or lung conditions. Any issues are optimised before the operation date is fixed.
Medication Review
Blood thinners (warfarin, aspirin, clopidogrel) are typically paused before surgery — usually 5–7 days beforehand, in liaison with your cardiologist or physician. Diabetic medications may need adjustment around the fasting period. Never stop any medication without your surgeon's specific guidance.
Consent & Discussion
The operation, its alternatives, specific risks (bile duct injury, bleeding, conversion to open, anaesthetic risks), and expected recovery are explained clearly. You have full opportunity to ask questions. Consent is documented formally — nothing is rushed.
Fasting & Admission
You will be asked to fast for 6 hours (solid food) and 2 hours (clear liquids) before your operation time. Most laparoscopic cholecystectomies are planned as day-surgery or one-night-stay procedures. Bring a list of your medications and any recent blood reports on the day.
What to Expect on the Day
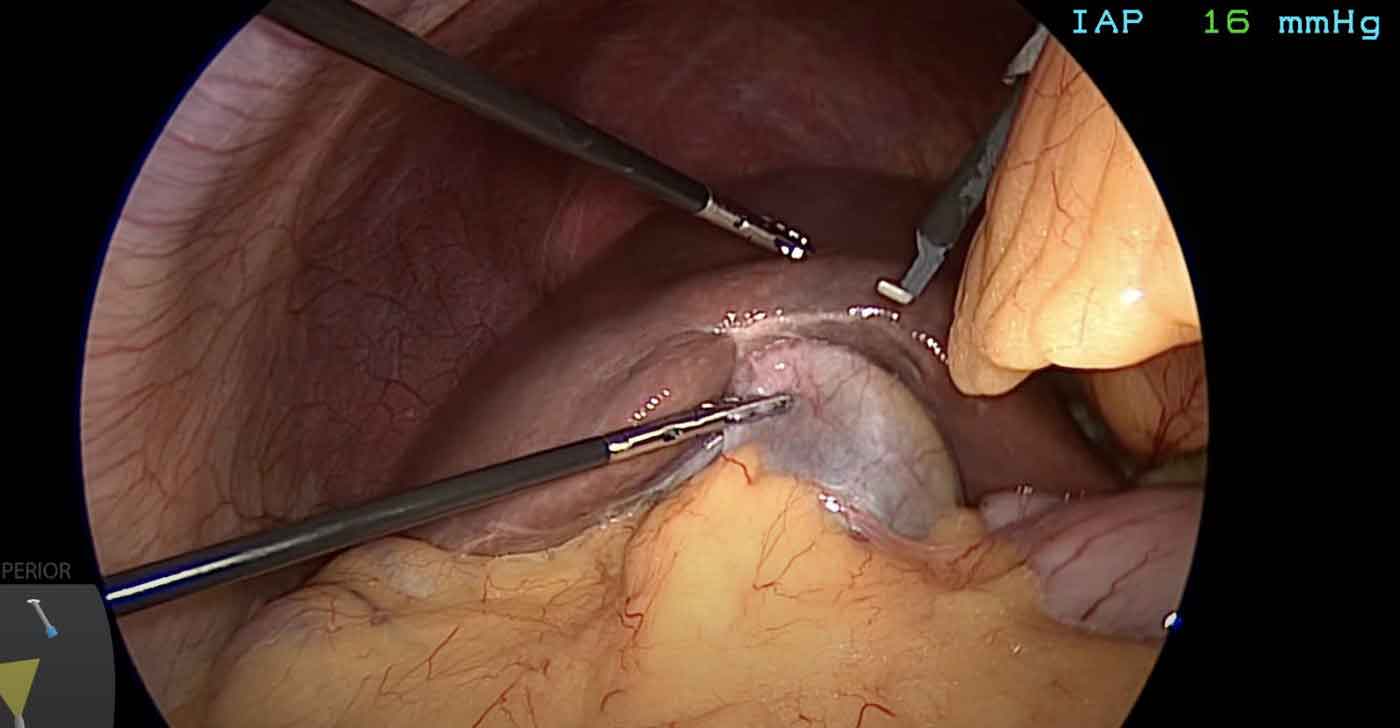
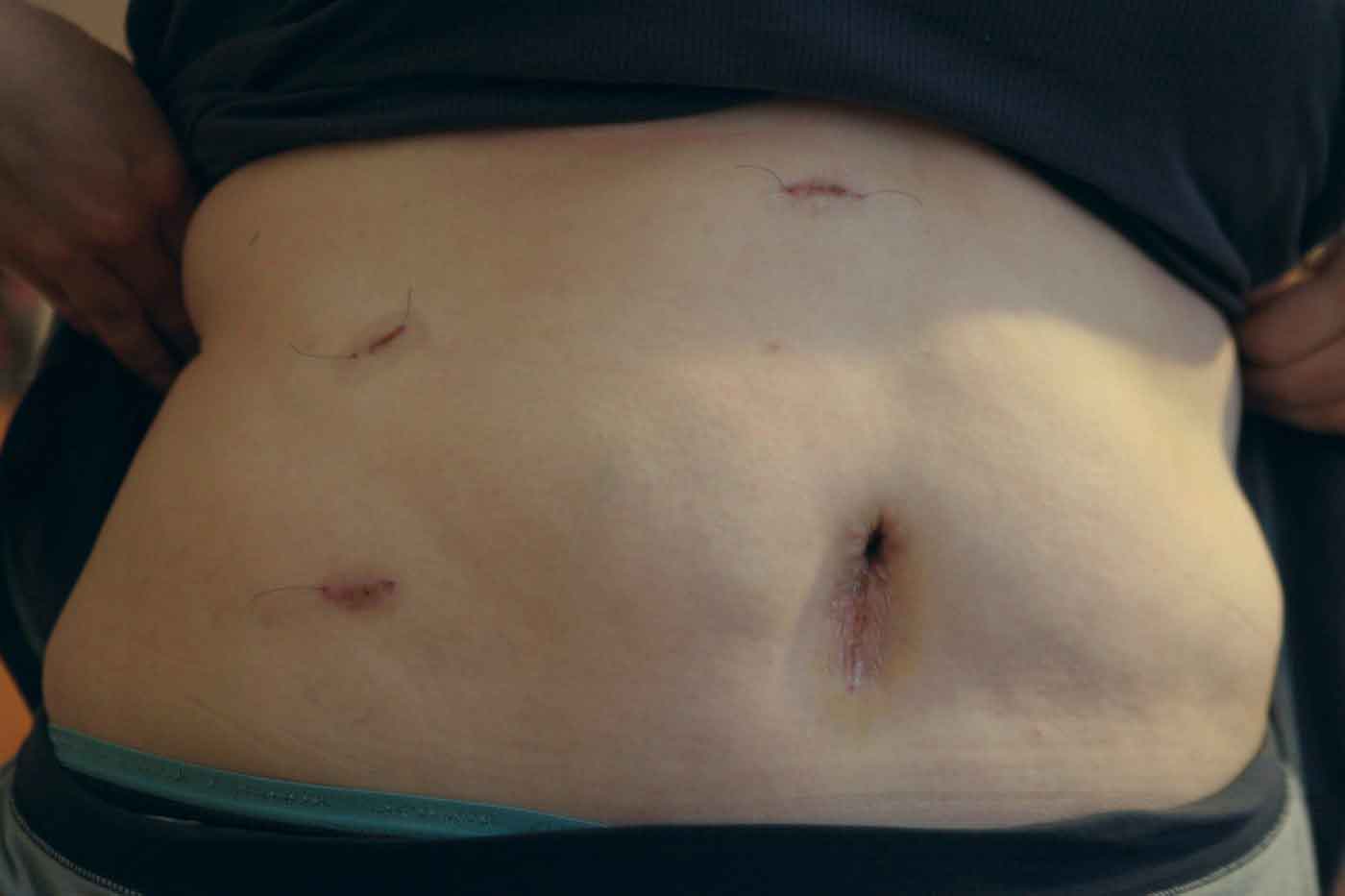
You are received in the ward, seen by the surgical and anaesthesia team, and shifted to the operating theatre when ready. The operation typically lasts 30–60 minutes. You wake up in the recovery room, then move to the ward. Most patients are walking within a few hours and eating a light meal by evening.
After Surgery — Questions & Answers
The questions patients ask most in the days and weeks after gallbladder surgery.
Who Is at Risk?
Gallstones do not strike randomly. Certain factors — many of them highly prevalent in the Indian population — significantly raise the likelihood of stone formation.
Female Sex
Women are three times more likely to develop gallstones than men. Indian data confirms: 5.59% prevalence in women vs. 1.99% in men. Oestrogen increases cholesterol secretion into bile; progesterone slows gallbladder emptying.
3× higher risk in womenPregnancy & Multiparity
Each pregnancy elevates oestrogen and progesterone, both of which promote stone formation. The gallbladder empties less efficiently during pregnancy, allowing bile to stagnate and crystallise. Risk rises with each successive pregnancy.
Hormonal Contraceptives & HRT
Oral contraceptive pills and hormone replacement therapy both raise oestrogen levels, increasing cholesterol concentration in bile and reducing gallbladder motility.
North Indian Diet
High intake of ghee, refined carbohydrates, saturated fat, and low dietary fibre — common in North Indian diets — promotes cholesterol supersaturation of bile. North Indians have 2–4× higher gallstone prevalence than South Indians.
2–4× higher in North IndiaDiabetes
Diabetes significantly impairs gallbladder motility, causing bile stasis and stone formation. Indian studies show diabetic patients have a 4.27× increased risk — particularly relevant given India's 101 million diabetics.
4.27× increased riskFamily History
A striking 69% of Indian gallstone patients report a positive family history. Genetic factors influence bile composition, gallbladder motility, and cholesterol metabolism — all of which contribute to stone formation.
69% have a family historyObesity & Rapid Weight Loss
Obesity increases cholesterol secretion into bile. Paradoxically, crash dieting or rapid weight loss (common in urban India) is equally dangerous — the gallbladder sits idle during fasting, allowing bile to concentrate and stones to form.
Age
Risk rises progressively after 40. In India, most symptomatic gallstone patients present between 40 and 60 years of age. Bile composition changes with age, and gallbladder contractility gradually declines.
Can Gallstones Be Prevented?
Not all gallstones are preventable — genetics and hormones play a role beyond our control. But lifestyle choices significantly influence your risk, and small consistent changes make a real difference.
Eat at Regular Times
Skipping meals allows bile to sit concentrated in the gallbladder for hours. Three regular meals — including breakfast — keep bile moving and reduce stasis.
Increase Dietary Fibre
Fruits, vegetables, whole grains, and legumes reduce bile cholesterol and speed intestinal transit. Replace refined carbohydrates and white rice with whole grains where possible.
Moderate Ghee & Saturated Fat
Ghee is not the enemy in small quantities, but daily high-volume use raises cholesterol in bile. Cook with less ghee; use plant-based oils for everyday cooking.
Stay Well Hydrated
Adequate fluid intake keeps bile dilute and less likely to crystallise. Aim for 8–10 glasses of water daily — more in summer or with physical work.
Maintain a Healthy Weight
Lose weight gradually — no more than 0.5–1 kg per week. Rapid weight loss sharply increases stone risk. Regular physical activity improves gallbladder motility directly.
Control Your Diabetes
Good glycaemic control reduces the gallbladder stasis associated with diabetes. If you are diabetic, a baseline abdominal ultrasound is worth discussing with your doctor.
Already have gallstones? These measures will not dissolve existing stones, but they reduce the risk of new ones forming after surgery and support your overall digestive health.