Intestinal Obstruction — Causes, Symptoms & Treatment in Chandigarh
One of the most common surgical emergencies. Dr. Rajeev Kapoor has extensive experience managing malignant, adhesive and all other forms of bowel obstruction — from conservative management to complex emergency surgery.
What Is Intestinal Obstruction?
Intestinal obstruction is a blockage that prevents food, fluid or gas from passing normally through the bowel. It is one of the most common surgical emergencies encountered in abdominal surgery — and one that demands prompt diagnosis and management.
The bowel can be obstructed anywhere along its length — from the small intestine (small bowel obstruction) to the large intestine or colon (large bowel obstruction). The blockage may be complete, where nothing passes through at all, or partial — known as a sub-acute obstruction — where contents still move through slowly.
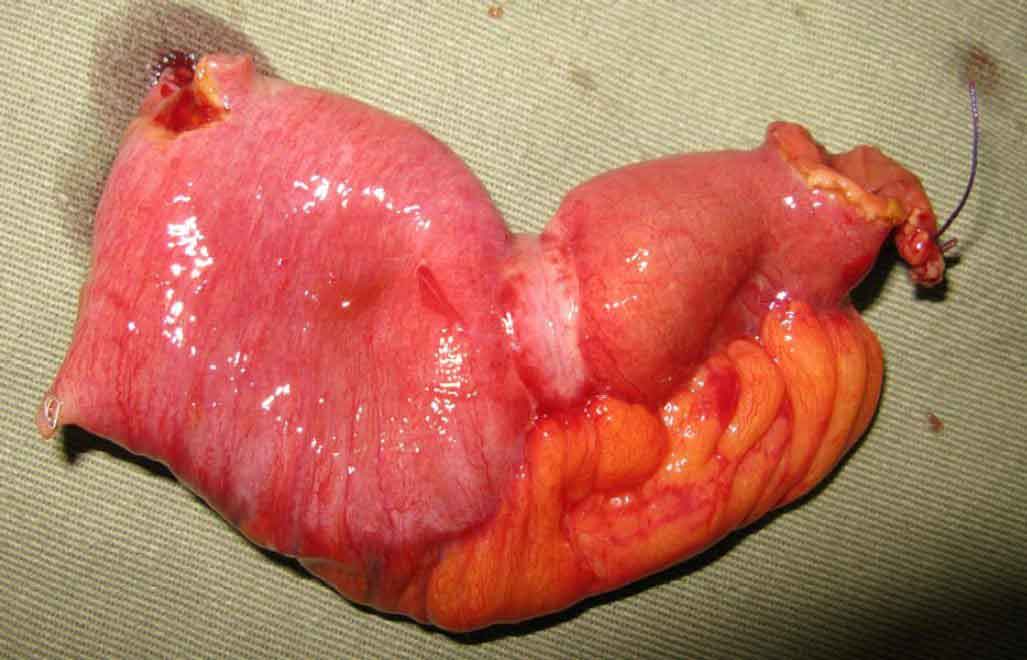
Mechanical vs Functional Obstruction
Most obstructions are mechanical — there is a physical blockage (a tumour, a band of scar tissue, or a twisted loop of bowel). A smaller number are functional (called ileus or pseudo-obstruction), where the bowel loses its ability to push contents forward even though there is no physical block. This page focuses primarily on mechanical obstruction.
💡 Important: If you have severe abdominal pain, a distended abdomen, vomiting, and inability to pass stools or wind, seek emergency care immediately. Bowel obstruction can become life-threatening within hours if not treated.
When the bowel is blocked, pressure builds up above the blockage. This can lead to bacterial overgrowth, fluid loss, reduced blood supply to the bowel wall, and eventually — if untreated — perforation and peritonitis (infection spreading inside the abdomen).
Causes & Types of Intestinal Obstruction
There is a wide range of causes of bowel obstruction. Understanding the cause is essential because each requires a different approach to management.
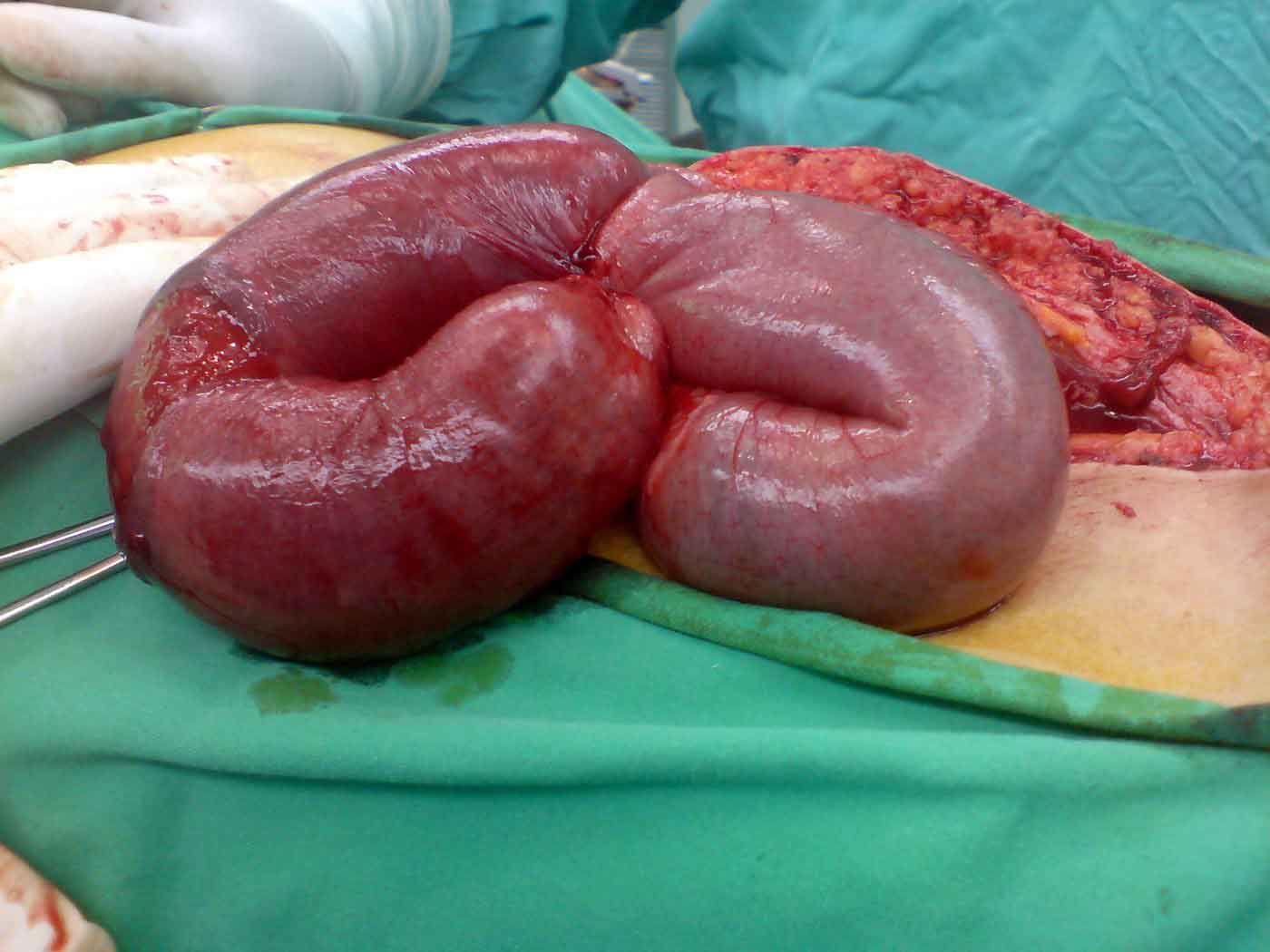
Malignant Obstruction (Cancer)
A growing tumour in the colon or rectum can narrow the bowel lumen until it blocks completely. This is the most common cause of large bowel obstruction in adults and often presents as an emergency.
📊 4 in 10 colorectal cancer patients first discover their cancer when obstruction brings them to hospital — often with no prior warning. This is why sub-acute symptoms must never be dismissed.
Malignant obstruction is the first presentation of colon cancer in a significant proportion of patients. The tumour may have been slowly narrowing the bowel for months before complete obstruction occurs. Treatment involves emergency surgery to relieve the obstruction, followed by definitive cancer management. In selected patients, an endoscopic stent may be placed to decompress the bowel, allowing elective surgery to be planned — a safer option than emergency resection.
Adhesive Obstruction (Scar Tissue)
Bands of scar tissue (adhesions) that form after previous abdominal surgery are the most common cause of small bowel obstruction. The scar bands trap and kink a loop of bowel.
Any previous abdominal operation — appendectomy, gynaecological surgery, bowel surgery, or even a caesarean section — can lead to adhesions. Most cases resolve with conservative treatment: rest, a tube through the nose to drain the stomach (nasogastric tube), and fluids through a drip. Post-operative patients are especially likely to be managed conservatively first, as adhesiolysis (surgery to divide scar bands) carries the risk of creating new adhesions and injuring the bowel during dissection.
Volvulus (Twisted Bowel)
The bowel twists on itself, cutting off both the lumen and the blood supply. Sigmoid volvulus is particularly common in India and seen frequently in the Chandigarh–Mohali region.
Sigmoid volvulus accounts for a substantial proportion of large bowel obstruction cases in India. The sigmoid colon — the S-shaped section of the colon — is especially prone to twisting when it is long and mobile. First-line treatment is endoscopic decompression (passing a tube through a sigmoidoscope or colonoscope to untwist the bowel). However, volvulus has a high recurrence rate and definitive surgery (sigmoid colectomy) is recommended once the patient has recovered from the acute episode.
Intussusception
One segment of bowel slides into the adjacent segment like a telescope collapsing. In children this is often idiopathic; in adults it usually has an identifiable cause such as a polyp or tumour.
In adults, intussusception rarely resolves on its own and surgery is usually required. A CT scan is important to identify the lead point (the underlying cause). If a cancer is found, formal cancer resection with lymph node clearance is performed. Benign causes such as a lipoma or polyp can be treated with a more limited resection.
Hernia
A loop of bowel trapped inside an abdominal hernia — inguinal, umbilical, incisional, or internal — can obstruct and strangulate. This requires urgent surgery.
An obstructed or strangulated hernia is one of the few causes of bowel obstruction that is immediately obvious on clinical examination — a tender, irreducible lump at the hernia site. If the blood supply to the trapped bowel has been cut off (strangulation), the bowel may already be dead (gangrenous) by the time of surgery. This requires not only hernia repair but also resection of the non-viable bowel and, often, formation of a stoma.
Other Causes
A wide range of other conditions can obstruct the bowel — including inflammatory bowel disease (Crohn's stricture), diverticular stricture, radiation stricture, gallstone ileus, and foreign bodies.
In Crohn's disease, repeated episodes of inflammation can lead to scar tissue and a narrowing (stricture) that eventually obstructs the bowel. Diverticular disease can cause similar scarring. Gallstone ileus is a rare condition where a gallstone erodes through the gallbladder into the bowel and becomes impacted at a narrow segment. Radiation stricture can develop months to years after radiotherapy for pelvic cancers. Each of these requires tailored management depending on the underlying cause.
Symptoms of Intestinal Obstruction
The symptoms of bowel obstruction depend on where the blockage is (small bowel vs large bowel), how complete it is, and whether the blood supply to the bowel has been affected.
⚠️ Warning Symptoms — Seek Emergency Care
- Severe, crampy abdominal pain that comes in waves
- Markedly distended (swollen) abdomen
- Vomiting — may become dark, foul-smelling (faeculent vomiting) in late stages
- Complete inability to pass stools or wind (absolute constipation)
- Fever, rapid heart rate, or collapse — signs of strangulation or perforation
Abdominal Pain
Crampy, colicky pain in waves — typically around the navel for small bowel and lower abdomen for large bowel obstruction. Pain becomes constant if strangulation sets in.
Vomiting
Early vomiting is typical of high small bowel obstruction. In large bowel obstruction, vomiting appears late — after the bowel above is very distended.
Abdominal Distension
Bloating and visible swelling of the abdomen. More marked in large bowel obstruction where a large volume of colon fills with gas and fluid.
Inability to Pass Stools or Wind
Absolute constipation — no flatus or stool at all — is the hallmark of complete mechanical obstruction. This is distinct from simple constipation.
Abnormal Bowel Sounds
High-pitched, tinkling bowel sounds may be heard (bowel working hard against the obstruction). Absence of sounds suggests ileus or peritonitis.
Fever & Tenderness
A rigid, tender abdomen with fever suggests strangulation or perforation — a surgical emergency requiring immediate operation.
🚨 When to Go to Hospital Immediately
Do not wait — bowel obstruction can become life-threatening within hours. Go to the emergency department if any of the following apply:
- 🔴 Sudden severe abdominal pain, especially if constant rather than coming in waves
- 🔴 Unable to pass any gas or stools for more than 24 hours
- 🔴 Vomiting that does not stop, or vomit that is dark and foul-smelling
- 🔴 Abdomen becoming progressively more swollen and hard
- 🔴 Fever, rapid pulse, or feeling faint alongside abdominal symptoms

Sub-Acute (Partial) Obstruction
Not all obstructions present as an emergency. A sub-acute or partial obstruction develops gradually and is easily missed — yet it is often the first sign of a serious underlying problem.
In sub-acute obstruction, the bowel is not completely blocked. Contents still move through, but slowly and with difficulty. The patient may experience weeks or months of symptoms before the situation becomes critical.
Dr. Kapoor's observation: Sub-acute obstruction is a common presentation in the Chandigarh–Mohali region. It is frequently the first sign of an underlying colorectal cancer that has been narrowing the bowel lumen gradually. Prompt investigation — rather than treating the symptoms alone — is essential.
🔄 Alternating Bowel Habits
Constipation alternating with loose stools or diarrhoea. The loose stool represents liquid contents squeezing past a partial blockage. This pattern is a red flag that must be investigated.
📈 Gradual Progression
Symptoms develop slowly — weeks or months of increasing bloating, cramping, and difficulty with bowel movements. Many patients attribute this to "gas" or "indigestion" before seeking help.
⚖️ Weight Loss & Appetite Change
Unexplained weight loss, reduced appetite or a feeling of incomplete emptying after a bowel movement (tenesmus) alongside bowel symptoms should always prompt investigation for cancer.
🩸 Rectal Bleeding
Blood in or on the stool alongside a change in bowel habit is a significant combination. Even small amounts of rectal bleeding with altered bowel habit should be assessed with a colonoscopy and CT scan.
How Sub-Acute Obstruction Is Investigated
A patient with these symptoms needs a CT scan of the abdomen and pelvis as the first investigation — this will identify most causes. A colonoscopy is then performed to directly visualise the inside of the bowel, take biopsies if a tumour is seen, and treat some causes (such as removing a polyp). If a cancer is found, staging scans are arranged and an MDT (multidisciplinary team) plan is made. Management is then semi-elective rather than emergency — which significantly improves outcomes.
Diagnosis
Prompt diagnosis is critical. The goals are to confirm obstruction, identify the level (small bowel vs large bowel), determine the cause, and assess whether the blood supply is compromised (strangulation).
Clinical Examination
History and examination are the starting point. Abdominal distension, previous surgical scars, a tender hernia site, abnormal bowel sounds, and rectal examination all provide important clues about the cause and severity.
Plain X-Ray Abdomen
Two views are taken: Erect and Supine. The erect X-ray shows air-fluid levels — horizontal fluid lines inside distended bowel loops that are a hallmark of obstruction. The supine view shows the full pattern and extent of bowel dilation, helping distinguish small bowel from large bowel obstruction. Together, they are the quickest first confirmation that obstruction is present.
CT Scan — Abdomen & Pelvis
A CT scan with contrast is the single most useful investigation. It identifies the site and level of obstruction, often reveals the cause (tumour, adhesion, volvulus), and can detect signs of strangulation or perforation.
Blood Tests
Full blood count, electrolytes, kidney function, inflammatory markers (CRP, WBC) and lactate. Raised lactate or white cell count with tenderness suggests possible strangulation — a surgical emergency.
Contrast Enhanced CT Scan
CE CT abdomen is the primary investigation. Gastrografin — given orally or via NGT — is not a routine challenge but has a dual role: it helps confirm and characterise the obstruction, and in adhesive small bowel obstruction can be directly therapeutic, helping the bowel resolve without surgery.
Colonoscopy
Used in sub-acute or partial obstruction when cancer is suspected. Provides direct visualisation, biopsy facility, and can treat some causes (volvulus decompression, stent placement in malignant obstruction).
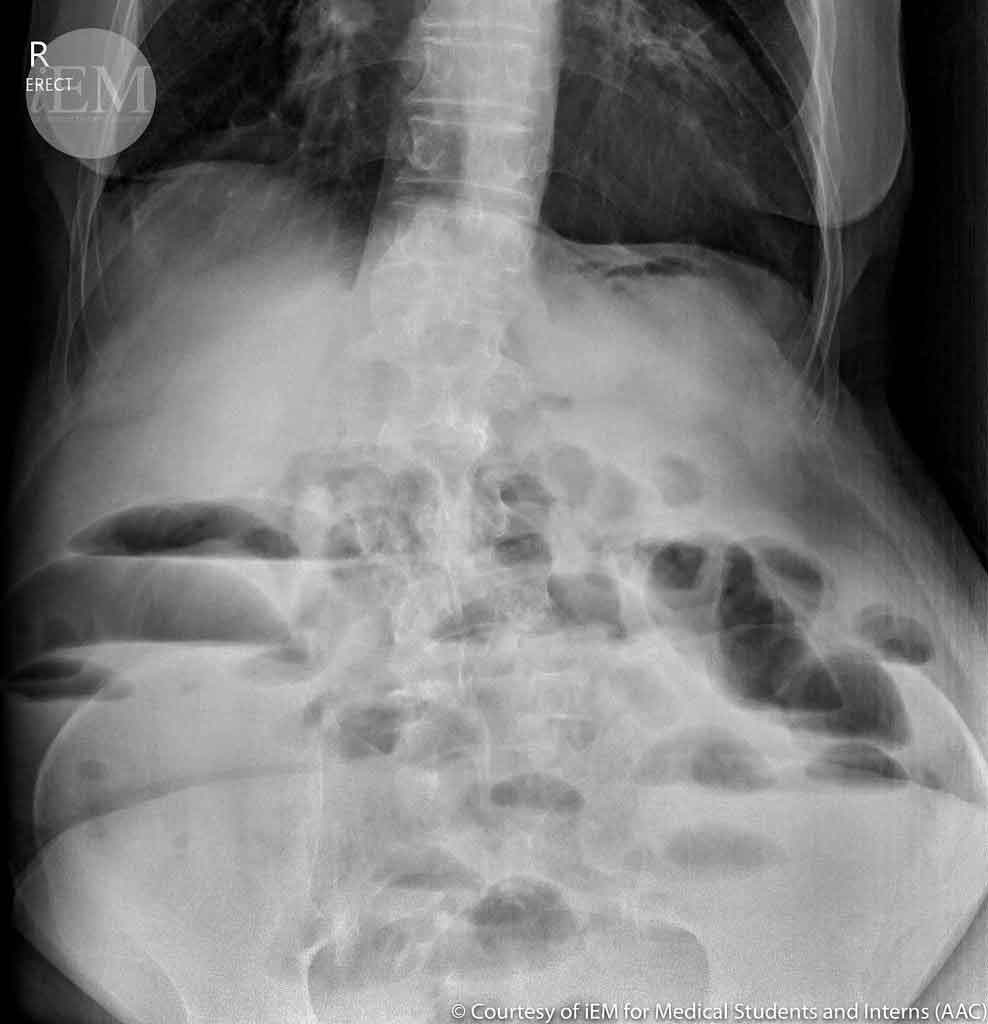
Erect X-ray — air-fluid levels visible in dilated bowel loops
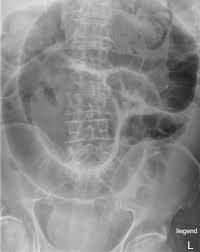
Supine X-ray — full extent of bowel dilation

Treatment
The treatment of bowel obstruction is not one-size-fits-all. The approach depends entirely on the cause, the patient's condition, and whether there are signs of compromised blood supply. Dr. Kapoor manages the full spectrum — from conservative care to complex emergency surgery.
Malignant Obstruction
When a colorectal cancer causes complete obstruction, emergency surgery is usually required. The blocked segment is resected and — in most emergency settings — a stoma (colostomy) is formed rather than a bowel join, which is safer in a distended, unprepared bowel.
In selected patients, an endoscopic self-expanding metal stent (SEMS) can be placed across the tumour to relieve the obstruction as a temporary measure ("bridge to surgery"), allowing the bowel to decompress and elective surgery to be performed under better conditions.
Adhesive Obstruction
The majority of cases — especially in post-operative patients — are managed conservatively first. This means hospital admission, drip fluids, nasogastric (NGT) tube to drain stomach secretions, bowel rest, and close monitoring.
Most post-operative adhesive obstructions resolve within 48–72 hours of conservative management. If there is no improvement, or if there are signs of strangulation, surgery to divide the adhesive bands (adhesiolysis) is performed — laparoscopically where possible.
Avoiding surgery is the goal — not just the first step. Operating on adhesions risks forming new scar bands and potentially restarting the same problem. We try hard not to operate unless the bowel is in danger.
Other Causes
Treatment is tailored to the underlying cause. Sigmoid volvulus is first treated endoscopically; definitive sigmoid resection follows electively. Obstructed hernia requires urgent surgery. Crohn's stricture may need resection or strictureplasty.
For functional obstruction (ileus), treatment is supportive — addressing the underlying cause (infection, electrolyte disturbance) and waiting for bowel function to recover.
Conservative Management — What It Involves
When surgery is not immediately needed, conservative management is initiated promptly. This is not "doing nothing" — it is an active treatment protocol that requires close monitoring:
Nil by Mouth & IV Fluids
The patient is kept nil by mouth (NBM) to rest the bowel. Intravenous fluids replace what would normally be absorbed — and correct the significant fluid losses that occur when bowel content accumulates above the obstruction.
Nasogastric (NGT) Tube
A fine tube passed through the nose into the stomach drains gastric secretions and swallowed air, reducing the pressure above the obstruction and relieving nausea and vomiting. Regular monitoring of NGT output guides the clinical picture.
Electrolyte Correction
Vomiting and fluid shifts can cause dangerous drops in potassium and sodium. Regular blood tests monitor electrolytes, which are replaced through the drip as needed.
Monitoring
Clinical examination is repeated frequently — looking for signs of deterioration. A worsening abdomen, rising lactate, increasing heart rate or fever despite conservative measures is an indication to proceed to surgery.
Contrast Enhanced CT Scan Abdomen
A CE CT scan of the abdomen is the primary investigation and is performed first in all cases. It confirms the diagnosis, identifies the level and cause of obstruction, and detects signs of strangulation or perforation. Gastrografin — when given orally or through the NGT — has an additional dual role: it helps characterise the obstruction further and in adhesive small bowel obstruction can be directly therapeutic, helping the obstruction resolve without surgery.
Endoscopic Stenting for Malignant Obstruction
What Is a SEMS?
A self-expanding metal stent is a mesh tube that is deployed across a tumour through a colonoscope. It expands to push the tumour walls apart and restore the lumen — allowing gas and stool to pass again within 24–48 hours, without any incision.
Bridge to Surgery
Placing a stent can avoid emergency surgery in a sick patient with a distended, unprepared bowel. It allows the obstruction to resolve, the bowel to decompress, the patient to recover, and nutritional status to improve — all before elective surgery is performed 2–4 weeks later. Elective surgery in a prepared bowel often achieves primary anastomosis (bowel join), avoiding a stoma. This is a significant quality-of-life benefit.
Palliation
In patients who are not fit for surgery, or whose cancer is too advanced for resection to help, a stent placed as definitive palliation can restore bowel function and avoid emergency surgery entirely.
Who Is It Suitable For?
Stenting is most effective for left-sided colon obstructions (sigmoid colon, descending colon). Technical success rates are high in experienced hands. It is not suitable for all cases — perforated tumours, very proximal obstruction, and emergency instability may mean surgery is the safer option. The decision is made case by case.
Surgery for Bowel Obstruction
When surgery is needed — whether as an emergency or elective procedure — the goal is to relieve the obstruction, remove any non-viable bowel, and restore continuity where safe to do so. Dr. Kapoor performs both laparoscopic and open procedures depending on the clinical situation.
Hartmann's Procedure
The standard emergency operation for malignant left-sided large bowel obstruction and many perforations. The blocked segment of colon is removed, the upper end is brought out as a colostomy, and the lower end (rectal stump) is closed off.
A second operation to join the bowel ends and reverse the colostomy can be considered once the patient has recovered from both the emergency and any cancer treatment needed.
Primary Resection & Anastomosis
In selected fit patients with a right-sided obstruction — or those undergoing elective resection after decompression — the bowel ends can be joined directly without forming a stoma. This is possible when the bowel is in good condition and the patient is stable.
Adhesiolysis (Dividing Adhesions)
When adhesive obstruction does not resolve with conservative management, surgery is performed to carefully divide the scar bands (adhesions) causing the blockage. Great care is taken to avoid injuring the adherent bowel loops during dissection.
Sigmoid Colectomy for Volvulus
After endoscopic decompression of an acute sigmoid volvulus, definitive surgical treatment is sigmoid colectomy — removing the redundant sigmoid colon to prevent recurrence. This is performed electively once the patient has recovered.
Stoma Formation
A stoma (colostomy or ileostomy) diverts the bowel contents to a bag on the abdomen. It may be formed temporarily — to protect a bowel join while it heals — or permanently, when rejoining is not safe or appropriate.
Hernia Repair
An obstructed or strangulated hernia requires urgent surgery. The trapped bowel is released, assessed for viability, and resected if gangrenous. The hernia is then repaired. Complex cases (incisional hernia with bowel resection) are among the most technically demanding emergency operations.
Recovery After Treatment
Recovery depends on whether you were treated conservatively or had surgery, the operation performed, and your overall health. Here is what to expect across the key aspects of recovery.
🏥 Hospital Stay
Conservative management typically requires 3–7 days in hospital until the bowel recovers. After elective surgery: 3–5 days. After emergency open surgery (e.g. Hartmann's): 7–12 days. Complex cases may be longer.
🥣 Resuming Eating
Sips of water are introduced once bowel sounds return and wind passes. Diet progresses gradually from clear fluids to light food. Most patients are eating normally before discharge. Nausea and slow return of appetite is common in the first week.
💊 Pain Management
Pain is managed with regular analgesia. After elective surgery, discomfort is usually mild. Emergency open surgery requires stronger pain relief for several days. Wound pain peaks on day 2–3 and improves steadily thereafter.
🚶 Activity & Return to Work
Short walks from day 1 or 2 post-surgery are encouraged to prevent clots and speed recovery. After elective surgery: light activity in 2–3 weeks, return to work in 3–4 weeks. After major emergency open surgery: 6–8 weeks before full activity.
👝 Stoma Care
If a stoma has been formed, a specialist stoma care nurse will teach you how to manage the bag, care for the skin around the stoma, and what to eat and avoid. Most patients manage the stoma confidently before discharge.
🔄 Follow-Up & Ongoing Care
A follow-up appointment at 4–6 weeks checks wound healing, bowel function, and reviews pathology results (if surgery was for cancer). If a cancer was found, oncology referral and staging will have been arranged during the admission.
Frequently Asked Questions
What is the most common cause of large bowel obstruction in India?
Colorectal cancer (malignant obstruction) is the most common cause of large bowel obstruction in adults in India. The tumour grows to block the colon lumen, often presenting as an emergency. Volvulus — particularly sigmoid volvulus — is another common cause seen across North India.
Can bowel obstruction be treated without surgery?
Yes — in many cases of adhesive obstruction (caused by scar bands from previous surgery), conservative management works well. This involves placing a nasogastric tube to drain secretions, giving fluids through a drip, resting the bowel, and monitoring closely. Most post-operative adhesive obstructions settle within 48–72 hours. However, if there is no improvement, or if there are signs of strangulation, surgery is necessary.
What is a sub-acute obstruction?
A sub-acute (or partial) obstruction means the bowel is not completely blocked — some contents can still pass through. Symptoms develop gradually over days or weeks and may include intermittent crampy pain, bloating, and alternating constipation and loose stools. This pattern is common as the first sign of an underlying colorectal cancer and must be investigated promptly with a CT scan and colonoscopy.
What happens if bowel obstruction is not treated?
Untreated bowel obstruction can progress to strangulation — where the blood supply to the bowel is cut off — leading to perforation, peritonitis (infection of the abdominal cavity), and life-threatening sepsis. Early diagnosis and treatment are essential to prevent these complications.
Will I need a colostomy after bowel obstruction surgery?
Not always. In planned or elective surgery, the bowel ends can often be joined directly (primary anastomosis) without a stoma. In emergency settings — particularly when the bowel is distended, inflamed, or contaminated — a temporary or permanent stoma may be safer. Temporary stomas are usually reversed after 8–12 weeks once healing is complete.
What is a Hartmann's procedure?
Hartmann's procedure is a commonly performed emergency operation for malignant large bowel obstruction or perforation. The blocked segment is removed, the upper end is brought out as a colostomy, and the lower end (rectal stump) is closed off. A second operation to restore bowel continuity can be considered when the patient has recovered, though not all patients are suitable candidates for reversal.
Can colon cancer cause intestinal obstruction?
Yes — a growing colorectal tumour can narrow the bowel lumen until it blocks completely. Patients may present acutely or sub-acutely (weeks of worsening constipation before complete blockage). Emergency surgery is often the first intervention, with cancer treatment continuing once the patient has recovered. This underlines why bowel cancer screening matters — detecting cancer before it obstructs gives far better treatment options.
How long is recovery after surgery for bowel obstruction?
Recovery depends on the cause and the type of surgery. After elective surgery, most patients go home in 3–5 days and return to normal activity in 2–3 weeks. After emergency open surgery for malignant obstruction, hospital stay is typically 7–12 days with 4–6 weeks of home recovery. If a stoma has been formed, stoma care training is provided before discharge.
Related Conditions & Procedures

Questions About Bowel Obstruction?
For more information about intestinal obstruction, its causes and treatment, contact your doctor. You can also contact Dr. Kapoor directly at Fortis Hospital, Sector 62, Mohali.
Contact Dr. Kapoor →For appointments or enquiries: Contact page | drrajeevkapoor.com